Video Link: https://vimeo.com/293539693
Video Download: Click Here To Download Video
Video Stream: Click Here To Stream Video
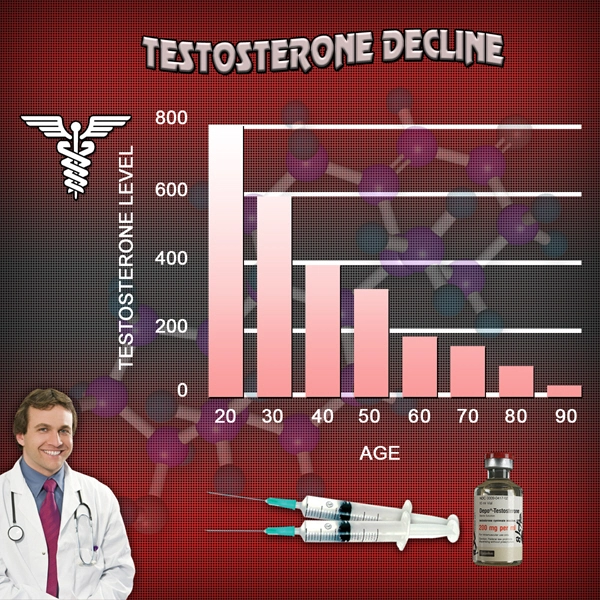
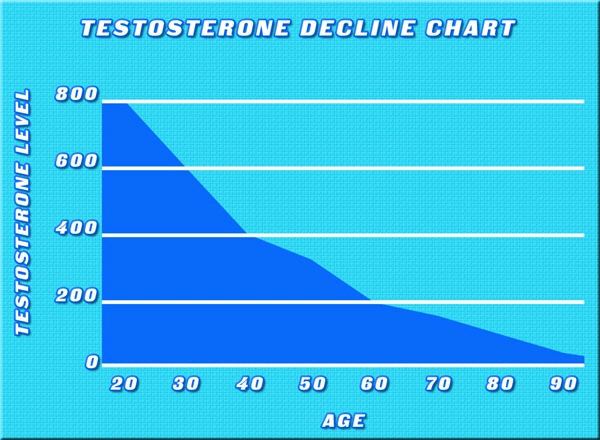
 Over the last ten years, there has been significant debate regarding the safety of Physician-Monitored Testosterone Replacement Therapy. The treatment is more popular today than it has ever been, but certain questions of safety have not been sufficiently resolved to promote the widespread use of the treatment. A collection of studies released in May of 2015 has brought us one step closer to that point.
Over the last ten years, there has been significant debate regarding the safety of Physician-Monitored Testosterone Replacement Therapy. The treatment is more popular today than it has ever been, but certain questions of safety have not been sufficiently resolved to promote the widespread use of the treatment. A collection of studies released in May of 2015 has brought us one step closer to that point.
One of the most critical contemporary concerns associated with Testosterone Therapy is how the treatment affects the Prostate. There have been some concerns that Testosterone Treatment can negatively impact the prostate, and lead to an increased risk of Prostate Cancer. Bio-Identical Testosterone has been previously associated with the release of a chemical known as PSA, or Prostate-Specific Antigen. In patients with Prostate Cancer, PSA levels are abnormally high, and it was hypothesized that the elevated PSA levels associated with Testosterone Therapy could be related to increased Prostate Cancer risk. New research suggests that these PSA counts have been overstated and that there is no significant correlation between Testosterone Levels and PSA Levels.
This did not, however, absolve Testosterone Therapy entirely of Prostate Cancer Risk, and further study was needed. These four studies, combined, provide strong evidence that the use of Testosterone for Hormone Replacement Therapy has no significant effect on prostate cancer risk.
The results of these studies will be revealed at the upcoming American Urological Association Conference.
Benefits of Testosterone for Male Patients with Low-T
These studies not only provide increased knowledge regarding the overall safety profile of Low-T Therapy, but they also provide more insight into the total benefits of Testosterone Treatment for men suffering from Andropause — or Age-Associated Testosterone Deficiency.
How Does Testosterone Benefit Patients?
 The following is a short list of ways that healthy Testosterone Levels Benefit Patients:
The following is a short list of ways that healthy Testosterone Levels Benefit Patients:
Increased Fertility – The body produces sperm as a direct result of the influence of Testosterone. Men with Testosterone Deficiency are more likely to have issues with fertility — the higher the deficiency, the lower the sexual potency.
Increased Libido – In both men and women, Testosterone is the primary trigger for sexual desire. When Testosterone Levels are too low, this leads directly to a reduced sex drive and passion for sexual pleasure.
Enhanced Sexual Ability – As Testosterone Levels decline, so does a man's ability to maintain a hard and healthy erection. Testosterone Deficiency leads to reduced sexual pleasure and is one of the primary causes of Erectile Dysfunction. Many men benefit from Testosterone Therapy without the need for Erectile Dysfunction Pills such as Viagra and Cialis.
Improved Red Blood Cell Count – Testosterone Deficiency is also associated with fatigue and lack of energy. This can be the result of inhibited Red Blood Cell Count associated with Abnormally Low Testosterone Levels. The cardiovascular system uses Red Blood Cells to transport oxygen through the body and facilitate energy production. For individual patients, this increased production of Red Blood Cells is not necessary and can be potentially problematic, in which case, blood donation, or other methods of relief can easily be performed.
Enhanced Muscle Mass and Strength – Testosterone is most notable, not only for its effect upon sexual function but because of its anabolic effects on the human body. Testosterone and other Steroids are often used and abused by professional athletes and weightlifters to improve their athletic performance, but this is not recommended, as the abuse of steroids can potentially have dangerous consequences. On the other hand, normalized Testosterone Levels are associated with healthy muscle mass and the promotion of strength. The decline in muscle mass and power associated with Testosterone Deficiency is another contributor to the weakness and fatigue related to the condition.
 Healthier Body Fat Composition – In addition to promoting strength, Testosterone also helps produce a leaner body. Testosterone is anabolic, which not only means that it builds muscle mass, but it encourages energy consumption as well. This is one reason why men need more calories on-average per day than women. As Testosterone Production drops due to Andropause, the body loses metabolism, and this results in increased body fat, particularly around the midsection, which is associated with an increased risk of heart and cardiovascular issues such as heart attack, cardiovascular disease, and stroke.
Healthier Body Fat Composition – In addition to promoting strength, Testosterone also helps produce a leaner body. Testosterone is anabolic, which not only means that it builds muscle mass, but it encourages energy consumption as well. This is one reason why men need more calories on-average per day than women. As Testosterone Production drops due to Andropause, the body loses metabolism, and this results in increased body fat, particularly around the midsection, which is associated with an increased risk of heart and cardiovascular issues such as heart attack, cardiovascular disease, and stroke.
Healthier Bone Density – In both men and women, the presence of healthy Testosterone Levels keeps the bones healthy. Testosterone Deficiency leads to a loss of bone mineral density that increases the risk of breaks, fractures, and osteoporosis. Women are more susceptible, and susceptible to this earlier because their lower innate Testosterone Production leaves them with weaker, less dense bone structure.
Testosterone Deficiency not the Only Cause of Low-T Associated Symptoms
Before turning to Testosterone, it is important to realize that Testosterone Deficiency is a deep-rooted disorder which shares many similar characteristics with other medical conditions. Never start taking Testosterone without undergoing the blood work and physical necessary to establish a clinical need for treatment.
Low-T Safety and Efficacy Study Details:
Study One: Testosterone Improves Cardiovascular Health in Older Patients
One study was conducted concerning evaluating the effectiveness and safety of Testosterone Therapy among elderly patients with Low-T. The long-term use of Testosterone has not been thoroughly evaluated, and this is one of the first significant studies to measure how safe the treatment is and how well it works when prescribed consistently for more than ten years. Researchers from the United States (Boston) and Germany (Bremerhaven) corroborated for this study and found that Physician-Prescribed Testosterone Therapy was beneficial concerning many symptoms in geriatric men with Low-T. Researchers found that these patients had an overall reduced risk of heart-related complications.
 This study used existing data to analyze 262 male patients with hypogonadism. These men took Intramuscular Testosterone once every three months for as long as eleven years. The following is a list of benefits that the patients experienced:
This study used existing data to analyze 262 male patients with hypogonadism. These men took Intramuscular Testosterone once every three months for as long as eleven years. The following is a list of benefits that the patients experienced:
- Reduced HbA1c Count
- Reduced Blood Sugar
- Improved BMI
- Weight Reduction
- Smaller Waist
- Lower Blood Pressure
- Suppressed Triglyceride Levels
- Healthier Cholesterol
Study Two: Testosterone Relieves Erectile Dysfunction Symptoms Among Diabetic Men and Improves Metabolic Function.
The same researchers conducted a second study which specifically evaluated patients with Diabetes that used Testosterone Therapy. They discovered that the same benefits listed in the previous research also led to an increase in sexual  function, and improved metabolism in these, particularly at-risk patients. Along with other recent studies, there is a growing body of evidence that Low-T Therapy can be a useful tool in the armory against Type-2 Diabetes.
function, and improved metabolism in these, particularly at-risk patients. Along with other recent studies, there is a growing body of evidence that Low-T Therapy can be a useful tool in the armory against Type-2 Diabetes.
Dr. Köhler, a lead researcher in these studies, is confident that Low-T Therapy with Testosterone Injections can be highly beneficial for many patients with unhealthy Testosterone Levels. Of course, the treatment won't be right for everyone, but he sees the potential for a considerable number of people to benefit.
Study Three: Testosterone Therapy Associated with Reduced Risk of Cardiovascular Complications
A third study assesses the risk of heart attack and stroke associated with Testosterone Therapy among men sixty-five and older. What they discovered was that Testosterone Injection Treatments did not lead to enhanced odds of experiencing medical issues such as pulmonary embolism, stroke, or heart attack. The study was produced by scientists from the Baylor College of Medicine and evaluated the medical records of men with untreated Low-T in comparison to men with Testosterone Deficiency that received Low-T Treatment. Two hundred patients were evaluated, separated into two of the mentioned groups.
What researchers discovered was that men that opted for Testosterone Therapy Treatment experienced improved mortality rates as compared to those that did not choose Low-T Therapy. On the other hand, Testosterone did not have any significant effect upon rates of Pulmonary Embolism or Heart Attack, for better or worse.
 Study Four: Testosterone Therapy, PSA, and Prostate Cancer Risk
Study Four: Testosterone Therapy, PSA, and Prostate Cancer Risk
This fourth study has not been fully processed yet, but so far, the evaluation shows that Testosterone Therapy Treatments do not appear to increase the chances of getting prostate cancer, nor do they necessarily lead to increased PSA-Count. The researchers in this study looked over the data of eighteen other studies, covering over five thousand cases of prostate cancer, and including almost twelve thousand controls. Researchers organized all patients by their Testosterone Levels and discovered that the risk of a patient getting prostate cancer had no significant correlation with their underlying Testosterone Levels. This was true of both endogenous, natural Testosterone and clinically-prescribed Testosterone Replacement.
Contact Us Today For A Free Consultation

Word Count: 1396