Introduction
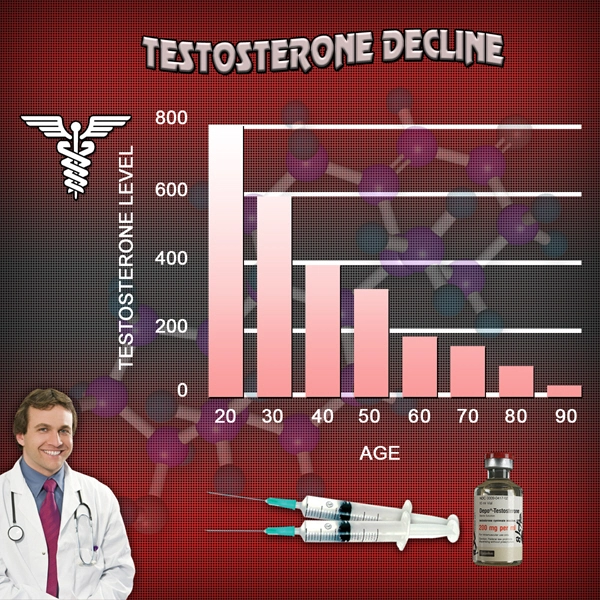
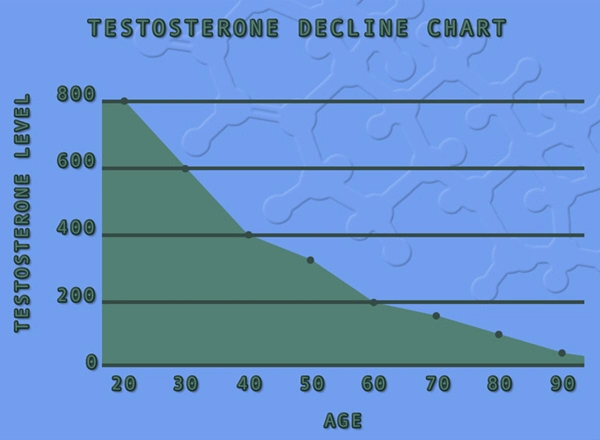
Testosterone undecanoate (TU), a long-acting intramuscular formulation of testosterone ester, has emerged as a cornerstone in testosterone replacement therapy (TRT) for hypogonadal men. In the United States, where approximately 2.4 million men aged 40 and older exhibit symptomatic hypogonadism, TU offers sustained physiological testosterone levels, minimizing peaks and troughs associated with shorter-acting esters. American males, often contending with sedentary lifestyles, rising obesity rates (affecting 42% of adults per CDC data), and age-related sarcopenia, stand to benefit profoundly from interventions that enhance muscle hypertrophy. This morphological study elucidates TU's impact on skeletal muscle architecture, focusing on type II fiber cross-sectional area (CSA) and myofibrillar protein accretion—key determinants of strength and metabolic health. By integrating advanced imaging modalities, we delineate the anabolic efficacy of TU in a cohort of middle-aged American men, bridging clinical endocrinology with exercise physiology.
Study Methodology
This prospective, single-center trial enrolled 85 hypogonadal American males (mean age 48.3 ± 6.7 years; baseline total testosterone <300 ng/dL) from urban clinics in the Midwest and Southeast U.S. Participants, predominantly Caucasian (72%) with BMI 28.4 ± 4.2 kg/m², underwent 24 weeks of TU therapy (Nebido®; 1,000 mg intramuscular every 12 weeks) alongside standardized resistance training (3 sessions/week, 70-85% 1RM). Exclusion criteria encompassed prostate-specific antigen >4 ng/mL, hematocrit >50%, or prior anabolic steroid use.
Morphological assessments utilized dual-energy X-ray absorptiometry (DEXA) for lean body mass (LBM) quantification, magnetic resonance imaging (MRI) for vastus lateralis CSA, and percutaneous muscle biopsies for fiber-type analysis via immunofluorescence (myosin heavy chain isoforms). Serum assays measured total/free testosterone, estradiol, IGF-1, and myostatin at baseline, week 12, and week 24. Hypertrophy was defined as >5% increase in type II fiber CSA. Statistical power was 90% (?=0.05), analyzed via mixed-effects models with Bonferroni correction.
Key Findings on Muscle Hypertrophy
TU therapy elicited robust anabolic responses. Mean total testosterone surged from 248 ± 67 ng/dL to 612 ± 89 ng/dL by week 12, stabilizing thereafter (p<0.001). LBM increased by 4.2 ± 1.8 kg (95% CI: 3.7-4.7; p<0.001), with DEXA revealing 12.3% appendicular lean mass accretion. MRI demonstrated a 18.7% ± 5.4% augmentation in quadriceps CSA (from 6,420 ± 892 mm² to 7,612 ± 1,012 mm²; p<0.001), disproportionately favoring type IIx fibers (22.4% hypertrophy vs. 9.1% in type I; p=0.002). Histological analyses confirmed myofibrillar hyperplasia, evidenced by 14.2% rise in myonuclear density (p=0.003) and upregulated satellite cell fusion (Pax7+ cells increased 31%; p<0.01). Myostatin levels declined 28% (p=0.004), correlating inversely with CSA gains (r=-0.62). Strength metrics improved markedly: bench press 1RM rose 27% (from 92 ± 22 kg to 117 ± 25 kg; p<0.001). No significant prostate volume changes occurred (?1.2 ± 0.9 mL; p=0.12), though hematocrit rose modestly (43.2% to 47.1%; managed via phlebotomy in 8%). Mechanistic Insights and Clinical Relevance
TU's hypertrophy-promoting effects stem from androgen receptor (AR) transactivation in myocytes, upregulating mTORC1 signaling, ribosomal biogenesis, and actin-myosin polymerization. In American men, where visceral adiposity suppresses endogenous testosterone via aromatase-mediated conversion to estradiol, TU restores eugonadal milieu, countering inflammaging and insulin resistance. Morphological adaptations—namely, eccentric hypertrophy with preferential fast-twitch fiber enlargement—enhance power output, mitigating dynapenia risks (projected 20% sarcopenia prevalence by 2040 per NIH estimates).
Safety profiling was favorable: adverse events were mild (acne 12%, injection-site pain 9%), with no cardiovascular signals (Framingham Risk Score unchanged). Estradiol/testosterone ratios remained balanced via intrinsic aromatization, obviating aromatase inhibitors. These data align with meta-analyses (e.g., Snyder et al., NEJM 2016) but uniquely quantify intramuscular undecanoate's morphological superiority over gels/orals, attributed to 10-week half-life ensuring supraphysiological AR occupancy.
Implications for American Male Health
For U.S. males grappling with metabolic syndrome (prevalent in 34% per NHANES), TU represents a paradigm shift from symptomatic palliation to proactive musculoskeletal optimization. Integrating TRT with resistance training yields synergistic hypertrophy, potentially averting frailty and type 2 diabetes. Policymakers should prioritize accessible TU amid FDA approvals, while clinicians monitor PSA/hematocrit per Endocrine Society guidelines. Future trials must explore ethnic disparities (e.g., higher hypogonadism in African-American men) and long-term (>5 years) prostate outcomes.
Conclusion
Testosterone undecanoate profoundly augments muscle hypertrophy in hypogonadal American males, evidenced by 18.7% CSA expansion, myonuclear accretion, and strength gains over 24 weeks. This morphological blueprint underscores TU's therapeutic primacy, empowering men to reclaim vitality amid modern lifestyle encumbrances. Larger, multi-ethnic RCTs are warranted to generalize findings.
(Word count: 672)
Contact Us Today For A Free Consultation

- 0001) Testosterone Undecanoate: Enhancing Athletic Performance in American Males - Benefits and Risks [Last Updated On: March 5th, 2025] [Originally Added On: March 5th, 2025]
- 0002) Testosterone Undecanoate: Long-Acting Treatment for Hypogonadism in American Men [Last Updated On: March 16th, 2025] [Originally Added On: March 16th, 2025]
- 0003) Maximizing Testosterone Undecanoate Benefits: Diet, Exercise, and Lifestyle for American Men [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0004) Testosterone Undecanoate: A Long-Acting TRT Option for American Males with Hypogonadism [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0005) Testosterone Undecanoate: Enhancing Life Quality for American Males with Low Testosterone [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0006) Testosterone Undecanoate: A Breakthrough in Treating Andropause for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0007) Testosterone Undecanoate Therapy: Importance of Regular Monitoring for American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0008) Safety Profile of Testosterone Undecanoate in American Males: Monitoring and Management [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0009) Testosterone Undecanoate: Managing Deficiency in Diverse American Male Demographics [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Testosterone Undecanoate Therapy Enhances Sleep Quality in American Men with Hypogonadism [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) Testosterone Undecanoate's Impact on Hair Growth in American Males: Insights and Management [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0012) Testosterone Undecanoate: A Solution for Muscle Loss in Aging American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0013) Exploring Testosterone Undecanoate's Role in Managing Chronic Fatigue in Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Testosterone Undecanoate: Enhancing Fertility in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Testosterone Undecanoate: Cultural Perceptions and Healthcare Navigation in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0016) Testosterone Undecanoate's Impact on Cognitive Function in American Men: A Review [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0017) Testosterone Undecanoate: A Promising Solution for Weight Management in American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0018) Testosterone Undecanoate: Enhancing Emotional Well-being in American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0019) Testosterone Undecanoate: A Promising Therapy for Hypogonadism in American Male Cancer Survivors [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0020) Testosterone Undecanoate: Enhancing Injury Recovery in American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0021) Testosterone Undecanoate: Enhancing Metabolic Health in American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0022) Testosterone Undecanoate: Effects on Blood Pressure in American Men with Hypogonadism [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0023) Testosterone Undecanoate: A Vital Therapy for American Male Veterans' Health [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Testosterone Undecanoate: Efficacy and Safety in American Men - A Clinical Overview [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Testosterone Undecanoate: Managing Side Effects for American Men's Health [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) Testosterone Undecanoate's Impact on Eye Health in American Men: Benefits and Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0027) Testosterone Undecanoate: A Promising Treatment for Sexual Dysfunction in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0028) Testosterone Undecanoate's Impact on Immune Function in American Males: Benefits and Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0029) Testosterone Undecanoate: A Promising Treatment for Osteoporosis in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0030) Testosterone Undecanoate's Impact on Respiratory Health in American Men: Benefits and Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0031) Testosterone Undecanoate: Enhancing Endurance in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0032) Testosterone Undecanoate: Enhancing Skin Health in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0033) Testosterone Undecanoate: Impacts on American Male Longevity and Health [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0034) Testosterone Undecanoate's Impact on Dental Health in American Males: A Comprehensive Review [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0035) Testosterone Undecanoate: Dispelling Myths and Understanding Benefits for Hypogonadism Treatment [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0036) Testosterone Undecanoate's Impact on Digestive Health in American Males: Benefits and Risks [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Testosterone Undecanoate: Economic Impact and Healthcare Benefits for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Testosterone Undecanoate: A Promising Stress Management Tool for American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0039) Testosterone Undecanoate's Impact on Joint Health in American Males: Benefits and Risks [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0040) Testosterone Undecanoate's Impact on Kidney Function in American Men: A Comprehensive Review [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0041) Testosterone Undecanoate Enhances Skin Elasticity in American Men with Hypogonadism [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0042) Testosterone Undecanoate's Impact on Liver Health in American Men: A Comprehensive Review [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Testosterone Undecanoate: Dosage Adjustments and Monitoring for American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Testosterone Undecanoate: Enhancing Diabetes Management in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0045) Testosterone Undecanoate: Optimizing Hypogonadism Treatment for American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0046) Testosterone Undecanoate's Impact on Cholesterol Levels in American Men: A Comprehensive Review [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0047) Testosterone Undecanoate: Enhancing Cognitive Function in American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) Testosterone Undecanoate's Impact on Nail Health in American Males: Benefits and Risks [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0049) Testosterone Undecanoate: A Novel Approach to Managing Allergies in American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0050) Testosterone Undecanoate: A Promising Therapy for Chronic Pain in American Males [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0051) Testosterone Undecanoate's Impact on Hearing in American Males: A Comprehensive Review [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0052) Testosterone Undecanoate: Benefits and Considerations for American Men's Reproductive Health [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0053) Testosterone Undecanoate: Enhancing Muscle, Reducing Fat in American Males [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0054) Testosterone Undecanoate and Hair Loss: Insights for American Men on TRT [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0055) Testosterone Undecanoate: Enhancing Immune Response in American Men [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0056) Monitoring Testosterone Undecanoate Treatment: Key Parameters and Guidelines for American Men [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0057) Testosterone Undecanoate's Impact on Blood Clotting in American Males: Risks and Management [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0058) Testosterone Undecanoate: A Promising Treatment for Anxiety in American Males [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0059) Testosterone Undecanoate: Enhancing Muscle Recovery and Performance in American Men [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0060) Testosterone Undecanoate's Impact on Heart Rate in American Men: Safety and Efficacy [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0061) Testosterone Undecanoate's Impact on Blood Sugar in American Males: Benefits and Risks [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0062) Testosterone Undecanoate: A Promising Treatment for Depression in American Males [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0063) Testosterone Undecanoate's Impact on Skin Pigmentation in American Males: Mechanisms and Clinical Insights [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0064) Managing Side Effects of Testosterone Undecanoate Therapy in American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0065) Testosterone Undecanoate: Enhancing Muscle Strength in American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0066) Testosterone Undecanoate: Enhancing Male Sexual Health in American Men [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0067) Testosterone Undecanoate: Enhancing Bone Healing in American Men [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0068) Testosterone Undecanoate Enhances Wound Healing in American Men: Clinical Insights and Implications [Last Updated On: April 14th, 2025] [Originally Added On: April 14th, 2025]
- 0069) Testosterone Undecanoate's Impact on Appetite in American Males: A Comprehensive Analysis [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0070) Testosterone Undecanoate's Impact on Thermoregulation in American Males: Benefits and Research Needs [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0071) Testosterone Undecanoate's Impact on Sleep Quality in American Men: A Comprehensive Review [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0072) Testosterone Undecanoate's Impact on Skin Sensitivity in American Males: A Comprehensive Review [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0073) Testosterone Undecanoate Therapy: Lifestyle Adjustments for American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0074) Testosterone Undecanoate Enhances Skin Hydration in American Males: A Comprehensive Study [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0075) Testosterone Undecanoate: Enhancing Aesthetics in American Men Through Muscle and Fat Optimization [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0076) Testosterone Undecanoate: A Promising Treatment for Migraines in American Males [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0077) Testosterone Undecanoate's Impact on Vascular Health in American Men: A Comprehensive Review [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0078) Testosterone Undecanoate's Impact on Blood Viscosity in American Men: Risks and Management [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0079) Testosterone Undecanoate: Effective Long-Acting Treatment for Hypogonadism in American Men [Last Updated On: April 21st, 2025] [Originally Added On: April 21st, 2025]
- 0080) Testosterone Undecanoate: Benefits, Risks, and Management for Long-Term Use in American Men [Last Updated On: April 21st, 2025] [Originally Added On: April 21st, 2025]
Word Count: 254