Introduction
Prostate health remains a cornerstone of men's wellness in the United States, where conditions such as benign prostatic hyperplasia (BPH), prostatitis, and prostate cancer affect millions annually. According to the American Cancer Society, over 288,000 new cases of prostate cancer are projected for 2023 alone, predominantly among men aged 65 and older. Concurrently, musculoskeletal decline—manifesting as sarcopenia (age-related muscle loss) and osteoporosis—poses significant morbidity risks. Recent epidemiological inquiries have illuminated intriguing associations between prostate pathologies and musculoskeletal integrity, suggesting shared pathophysiological pathways influenced by androgens, inflammation, and lifestyle factors. This article synthesizes evidence on how muscle and bone health intersect with prostate conditions in American males, underscoring implications for preventive strategies and holistic management.
Epidemiology of Prostate Disorders in American Males
Prostate conditions exhibit high prevalence in the U.S. demographic. BPH impacts approximately 50% of men in their 60s and up to 90% by age 85, per data from the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). Prostate cancer, the second leading cause of cancer death in American men, disproportionately burdens African American males, with incidence rates 70% higher than in white counterparts. Symptoms range from lower urinary tract issues to metastatic complications. Risk factors include age, genetics, obesity, and metabolic syndrome, which also predispose individuals to musculoskeletal frailty. Longitudinal studies, such as those from the Prostate, Lung, Colorectal, and Ovarian (PLCO) Cancer Screening Trial, reveal that sedentary lifestyles—prevalent in 25% of U.S. adult males per CDC reports—exacerbate both prostate enlargement and muscle atrophy.
Musculoskeletal Health Dynamics in Aging Men
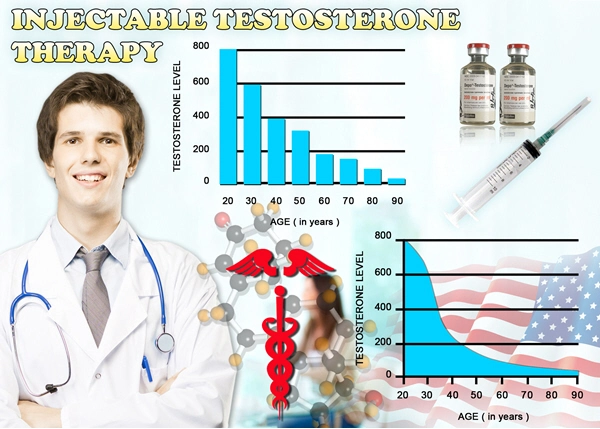
Musculoskeletal health in American males deteriorates progressively post-40, driven by declining testosterone levels. Sarcopenia affects up to 30% of community-dwelling men over 60, characterized by appendicular skeletal muscle mass loss exceeding 3% annually. Osteoporosis, often underdiagnosed, manifests in 2 million U.S. men, with fragility fractures costing $19 billion yearly (National Osteoporosis Foundation). Dual-energy X-ray absorptiometry (DEXA) scans frequently uncover low bone mineral density (BMD) in men on androgen deprivation therapy (ADT) for prostate cancer, where bone loss accelerates by 2-4% per year. Physical inactivity, nutritional deficits in vitamin D and calcium, and chronic inflammation further compound these vulnerabilities, mirroring prostate disease risk profiles.
Associations Between Prostate Conditions and Musculoskeletal Decline
Emerging research delineates robust correlations. A 2022 cohort study in the *Journal of Urology*, analyzing 5,000 U.S. veterans, found men with low grip strength (a sarcopenia proxy) had a 1.8-fold increased risk of clinically significant prostate cancer (Gleason score ?7). Similarly, the Osteoporotic Fractures in Men Study (MrOS) reported that frailty indices predicted BPH progression independently of age. ADT, prescribed to 50% of advanced prostate cancer patients, induces profound musculoskeletal sequelae: sarcopenic obesity in 20-30% and vertebral fractures in 10-20%. Inflammatory cytokines like IL-6, elevated in both prostatitis and osteoporosis, mediate this nexus. Metabolic syndrome, afflicting 34% of U.S. men (CDC), links visceral adiposity to prostate volume expansion and myocellular apoptosis.
Pathophysiological Mechanisms
Hormonal dysregulation underpins these interlinks. Testosterone deficiency, prevalent in 40% of men over 45, impairs prostate epithelial integrity while diminishing muscle protein synthesis via reduced IGF-1 signaling. Estrogen-androgen imbalance from aromatase activity in adipose tissue promotes osteoclast activation, eroding BMD and fostering prostate stromal proliferation. Chronic low-grade inflammation, quantified by C-reactive protein levels, bridges prostatitis to sarcopenia through NF-?B pathways. Oxidative stress from mitochondrial dysfunction in prostate cells parallels myonuclear apoptosis. Genome-wide association studies (GWAS) identify shared loci, such as FOXO3, regulating longevity and tissue resilience in both systems.
Clinical Implications and Preventive Strategies
For American males, integrated screening is imperative. Urologists should incorporate frailty assessments—like the Short Physical Performance Battery—alongside prostate-specific antigen (PSA) testing. Resistance training (3 sessions/week) and weight-bearing exercises mitigate ADT-induced losses, as evidenced by a randomized controlled trial in *JAMA Oncology* showing 5% BMD gains. Pharmacotherapies include bisphosphonates (e.g., zoledronic acid) for high-risk ADT patients and selective androgen receptor modulators (SARMs) for sarcopenia. Nutritional interventions—emphasizing 1,200 mg daily calcium, 2,000 IU vitamin D, and leucine-rich proteins—align with American Urological Association guidelines. Lifestyle modifications, targeting the 70% of U.S. men exceeding sedentary thresholds, yield dual benefits: a 25% prostate cancer risk reduction and enhanced muscle mass per meta-analyses.
Conclusion
The confluence of prostate and musculoskeletal health in U.S. males heralds a paradigm shift toward multidisciplinary care. By addressing shared risk vectors—hormonal flux, inflammation, and sedentariness—clinicians can avert compounded morbidities. Future prospective trials, leveraging wearable biosensors for real-time monitoring, promise refined risk stratification. Empowering American men with actionable insights fosters resilience across these interconnected domains, optimizing quality-adjusted life years in an aging populace.
(Word count: 672)
Contact Us Today For A Free Consultation

- 0001) Prostate Health in Aging American Men: BPH, Cancer, and Lifestyle Management [Last Updated On: March 1st, 2025] [Originally Added On: March 1st, 2025]
- 0002) Prostate Health Essentials: Risks, Prevention, and Screening for American Men [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0003) Understanding Benign Prostatic Hyperplasia: Symptoms, Diagnosis, and Management in American Men [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0004) Prostate Health and Cancer: The Crucial Role of Family History in American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0005) Exercise Regimen for Optimal Prostate Health in American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0006) Navigating Life After Prostate Cancer: Health, Well-being, and Survivorship Strategies [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0007) Dietary Strategies for Enhancing Prostate Health in American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0008) Prostate Cancer Screening: Controversies, Guidelines, and Future Directions [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0009) Prostate Cancer Treatments: Understanding and Managing Side Effects for American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Exercise as a Key to Prostate Health for American Males: Benefits and Recommendations [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) Prostate Health and Heart Disease: Understanding the Connection and Risks for American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0012) Prostate Cancer's Psychological Impact on American Men: Diagnosis to Recovery [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0013) Prostate Health: Understanding Symptoms, Seeking Care, and Maintaining Wellness in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Prostate Cancer Stages and Grades: A Comprehensive Guide for American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Vitamin D's Role in Prostate Health: Insights and Recommendations for American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0016) Environmental Factors and Prostate Health: Risks and Mitigation Strategies for American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0017) Hydration's Vital Role in Prostate Health for American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0018) Avoid These Foods for Better Prostate Health in American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0019) Palliative Care's Vital Role in Enhancing Prostate Cancer Management and Quality of Life [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0020) Chemotherapy's Role in Managing Prostate Cancer: Efficacy and Quality of Life in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0021) Active Surveillance: A Tailored Approach to Managing Low-Risk Prostate Cancer [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0022) Prostate Cancer and Cryotherapy: Benefits, Risks, and Management for American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0023) Prostate Cancer's Impact on Fertility: Treatments and Preservation Options [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Prostate Cancer and Radiation Therapy: Efficacy, Side Effects, and Future Advances [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) HIFU: A Minimally Invasive Hope for Prostate Cancer Treatment [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) Prostate Cancer Treatment: Understanding Brachytherapy's Benefits and Procedure [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0027) Sleep's Crucial Role in Prostate Health for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Prostate Cancer Support Groups: Emotional, Educational, and Practical Benefits for Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Immunotherapy: A Promising Frontier in Prostate Cancer Treatment for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Omega-3 Fatty Acids: A Promising Approach to Prostate Health in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) CyberKnife: Advanced, Non-Invasive Prostate Cancer Treatment for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Alcohol Consumption and Prostate Health: Insights and Recommendations for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0033) Proton Therapy: A Targeted Approach to Treating Prostate Cancer in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0034) Targeted Therapy: Revolutionizing Prostate Cancer Treatment for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0035) Stress Impact on Prostate Health: Management Strategies for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0036) Heavy Metals and Prostate Health: Risks and Prevention Strategies for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0037) Photodynamic Therapy: A Promising Treatment for Prostate Cancer in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0038) Hormone Therapy: Managing Prostate Cancer and Enhancing Life Quality [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0039) Pesticides and Prostate Health: Risks, Mechanisms, and Prevention for American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0040) Green Tea Benefits for Prostate Health in American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0041) Antioxidants: Key to Prostate Health and Disease Prevention in American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0042) Selenium's Role in Prostate Health: Benefits and Optimal Intake for American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0043) Air Pollution's Emerging Link to Prostate Health Issues in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Lycopene's Role in Enhancing Prostate Health: Benefits and Dietary Sources [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0045) Prostate Cancer Management: Understanding Watchful Waiting and Its Benefits [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0046) Prostate and Bone Health: Understanding the Connection and Management Strategies [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0047) Zinc's Vital Role in Prostate Health for American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0048) Plastics and Prostate Health: Risks, Research, and Mitigation Strategies for American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0049) Chronic Inflammation's Impact on Prostate Health in American Males: Risks and Management [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0050) Chemoprevention Strategies for Prostate Cancer: Agents and Clinical Insights [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0051) Prostate Cancer Surgery: Benefits, Risks, and Comprehensive Management for American Men [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0052) EMFs and Prostate Health: Risks, Mechanisms, and Mitigation Strategies for American Males [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0053) Vitamin E's Role in Prostate Health: Benefits and Considerations for American Males [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0054) Robotic Surgery for Prostate Cancer: Benefits and Procedure for American Men [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0055) Prostate Cancer: Focal Therapy's Role in Minimizing Side Effects for American Men [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0056) Cruciferous Vegetables: A Dietary Approach to Enhancing Prostate Health in American Males [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0057) Endocrine Disruptors and Prostate Health: Risks, Exposure, and Mitigation Strategies [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0058) Industrial Chemicals and Prostate Health: Risks and Prevention Strategies [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0059) Soy Benefits for Prostate Health: Reducing Cancer Risk and Managing BPH [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0060) Laparoscopic Prostatectomy: Minimally Invasive Cancer Treatment and Recovery Insights [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0061) Adjuvant Therapy's Role in Managing Prostate Cancer Among American Men [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0062) Salvage Therapy: A Second Chance for American Men with Prostate Cancer Recurrence [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0063) Neoadjuvant Therapy in Prostate Cancer: Insights for American Men's Health [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0064) Medications and Prostate Health: Impacts, Monitoring, and Holistic Management for American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0065) Flaxseed: A Natural Approach to Enhancing Prostate Health in American Males [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0066) Pomegranates: A Natural Approach to Enhancing Prostate Health in American Males [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0067) Palliative Surgery for Prostate Cancer: Enhancing Quality of Life for American Men [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0068) Bisphosphonates: Enhancing Bone Health in Metastatic Prostate Cancer Management [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0069) Shift Work's Impact on Prostate Health: Risks and Mitigation Strategies [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0070) Ginger's Potential Benefits for Prostate Health in American Males [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0071) Radium-223: A Targeted Therapy for Advanced Prostate Cancer in American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0072) Heavy Physical Work's Impact on Prostate Health in American Males [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0073) Turmeric's Role in Enhancing Prostate Health: Benefits and Clinical Insights [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0074) Abiraterone: Advancing Treatment for Metastatic Prostate Cancer in American Men [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0075) Denosumab: A Promising Treatment for Prostate Cancer with Bone Metastases [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0076) RANK Ligand Inhibitors: A New Hope in Managing Advanced Prostate Cancer [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0077) Prostate Health Risks and Strategies for Long-Haul Truckers [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0078) Enzalutamide: A New Hope in Prostate Cancer Treatment for American Men [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0079) Prostate Cancer: Symptoms, Diagnosis, Treatment, and Proactive Health for American Males [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0080) Tomatoes and Prostate Health: The Role of Lycopene in Cancer Prevention [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
Word Count: 738