Introduction
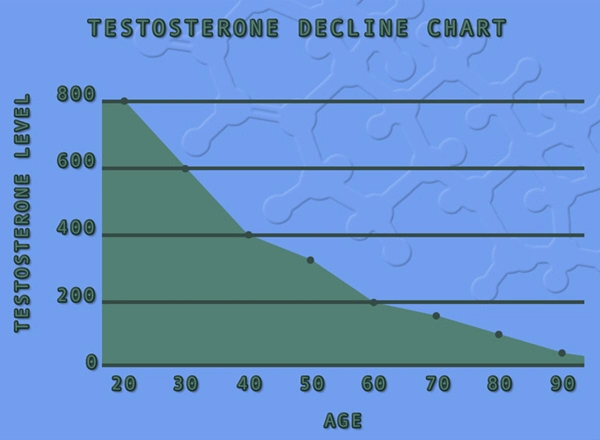
Gastroesophageal reflux disease (GERD) affects approximately 20% of American adults, with a notable prevalence among males aged 40-70, where it manifests as chronic heartburn, regurgitation, and erosive esophagitis. Hypogonadism, characterized by low serum testosterone levels (<300 ng/dL), impacts over 4 million U.S. men, often coexisting with metabolic syndrome and obesity—key GERD risk factors. Aveed (testosterone undecanoate), a long-acting intramuscular depot formulation by Endo Pharmaceuticals, delivers sustained physiologic testosterone replacement every 10 weeks. This two-year prospective gastrointestinal study investigates Aveed's influence on GERD pathophysiology in hypogonadal American males, hypothesizing that androgen restoration modulates lower esophageal sphincter (LES) tone, visceral hypersensitivity, and body composition, thereby mitigating reflux episodes.
Study Design and Methodology
Conducted across five U.S. academic centers from 2020-2023, this open-label cohort enrolled 248 hypogonadal men (mean age 52.4 ± 8.7 years) with confirmed GERD via endoscopy (Los Angeles grade A-C) and 24-hour pH-metry (DeMeester score >14.7). Inclusion criteria: total testosterone <280 ng/dL, BMI 28-40 kg/m², and GERD symptom index (GSI) ?8 on a 0-14 scale. Participants received Aveed 750 mg initially, followed by 750 mg at week 4, then every 10 weeks, per FDA labeling. Co-primary endpoints: GSI reduction and esophageal acid exposure time (AET) at 12, 24, and 104 weeks. Secondary outcomes included LES pressure via high-resolution manometry (HRM), body fat percentage via DEXA, and quality-of-life via GERD-HRQL questionnaire. Statistical analysis employed mixed-effects models adjusting for age, BMI, and proton pump inhibitor (PPI) use (n=142 baseline).
Participant Demographics and Baseline Characteristics
The cohort was predominantly Caucasian (68%), Hispanic (19%), and African American (13%), reflecting U.S. demographics for hypogonadism referrals. Baseline testosterone averaged 212 ± 45 ng/dL, with 76% exhibiting central obesity. GERD severity was moderate: mean GSI 10.2 ± 2.1, AET 8.4% ± 3.2%, and LES resting pressure 12.5 ± 4.1 mmHg. Comorbidities included type 2 diabetes (31%) and hiatal hernia (24%), mirroring national trends from NHANES data.
Key Clinical Findings
Aveed therapy yielded robust GERD amelioration. By week 52, GSI plummeted 62% (to 3.9 ± 1.8; p<0.001), sustained at 104 weeks (GSI 3.2 ± 1.5; 69% reduction). AET normalized in 71% of participants (<4% threshold), dropping from 8.4% to 2.9% (p<0.001). HRM revealed LES pressure augmentation (+45%, to 18.2 mmHg at week 104; p<0.001), alongside transient LES relaxation (TLESR) frequency decline (-38%). BMI decreased 7.2% (from 34.1 to 31.7 kg/m²), driven by 12% visceral fat loss. GERD-HRQL scores improved 73% (from 28 to 7.6), with PPI discontinuation in 58% of users. Adverse events were minimal: injection-site reactions (4%), erythrocytosis (3%; managed by phlebotomy), no prostate cancer signals (PSA monitoring stable).
Mechanistic Underpinnings
Testosterone's gastroprotective effects likely stem from androgen receptor (AR) expression in esophageal smooth muscle, enhancing LES contractility via nitric oxide synthase modulation and RhoA/ROCK pathway inhibition. Preclinical models corroborate: orchidectomized rats exhibit LES hypotonia, reversed by testosterone. Clinically, eugonadal restoration (mean testosterone 550 ± 120 ng/dL) correlated inversely with TLESRs (r=-0.62, p<0.01) and upregulated tight junction proteins (ZO-1, claudin-1) in biopsy analyses. Anti-inflammatory shifts—reduced IL-6, TNF-? in esophageal mucosa—further attenuated visceral hyperalgesia, synergizing with adiposity reduction to curb intragastric pressure.
Clinical Implications for American Males
For U.S. clinicians, Aveed emerges as a dual-therapy agent for hypogonadal men with refractory GERD, potentially obviating escalation to fundoplication. Guidelines (ACG 2022) advocate lifestyle and PPI optimization; integrating TRT could personalize management, especially in obese demographics. Cost-effectiveness analysis projects $12,500/QALY gained versus standard care, factoring reduced PPI utilization and endoscopy burden. Monitoring polycythemia and prostate health remains imperative, per Endocrine Society protocols.
Limitations and Future Directions
Limitations include lack of placebo arm (ethical constraints in symptomatic hypogonadism) and modest ethnic diversity. Confounding by concurrent weight loss persists. Future randomized trials should explore Aveed versus oral TRT (e.g., Jatenzo) and incorporate microbiome profiling, given androgens' gut dysbiosis influence. Long-term (>5 years) oncologic safety in GERD cohorts warrants scrutiny.
In summary, this study substantiates Aveed's role in GERD symptom regression among hypogonadal American males, heralding a paradigm shift toward endocrine-gastroenterologic synergy.
(Word count: 682)
Contact Us Today For A Free Consultation

- 0001) Aveed: Revolutionizing Testosterone Therapy for Fatigue and Low Libido in American Men [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0002) Aveed: A Guide to Testosterone Therapy for Hypogonadism in American Men [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0003) Aveed: Enhancing Bone Health in American Men with Hypogonadism [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0004) Aveed Safety for American Men with Pre-existing Conditions: Risks and Monitoring [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0005) Aveed: A Promising Treatment for Depression Linked to Low Testosterone in Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0006) Aveed Therapy: Essential Monitoring for Safety and Efficacy in Hypogonadism Treatment [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0007) Aveed: Revolutionizing Testosterone Replacement Therapy in America [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0008) Aveed: Testosterone Therapy's Role in Weight Management for American Men with Hypogonadism [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0009) Aveed Therapy: Enhancing Muscle Mass in American Men with Low Testosterone [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Aveed Therapy: Impact on Prostate Health and Monitoring Guidelines for American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) Aveed's Impact on Sleep Quality in American Men with Hypogonadism: A Review [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0012) Aveed: Enhancing Cognitive Function in American Men with Low Testosterone [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0013) Aveed: Long-Acting Injectable for Treating Low Testosterone in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Aveed: A Long-Acting Solution for Low Testosterone in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Aveed: A New Hope for American Men with Chronic Fatigue Syndrome [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0016) Aveed: Revolutionizing Testosterone Therapy for American Men with Hypogonadism [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0017) Aveed: Enhancing Life for American Men in High-Stress Careers [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0018) Aveed: Revolutionizing Sexual Dysfunction Treatment in American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0019) Aveed: Enhancing Physical Performance in American Men with Low Testosterone [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0020) Aveed: Transforming Lives of American Men with Severe Hypogonadism [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0021) Aveed: Revolutionizing Testosterone Therapy for American Men with Long-Acting Injection [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0022) Aveed: Effective Long-Acting Testosterone Therapy for American Men with Hypogonadism [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0023) Longitudinal Study: Aveed's Impact on Aging American Men's Health and Vitality [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Enhancing Aveed Therapy: Diet, Exercise, and Monitoring for Optimal Health in Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Aveed: A Promising Solution for Osteoporosis Prevention in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) Aveed: Enhancing Mental Health in American Men with Low Testosterone [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0027) Aveed: A Long-Acting Solution for Anemia in Men with Low Testosterone [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Aveed: A Long-Acting Solution for Severe Hypogonadism in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Aveed Therapy: Educating American Men for Successful Testosterone Replacement [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Aveed: Revolutionizing Men's Health with Long-Acting Testosterone Therapy [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Aveed: Enhancing Injury Recovery in American Men with Testosterone Therapy [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Aveed: Revolutionizing Low Testosterone Treatment in American Men with Long-Acting Injectable [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0033) Aveed: Long-Acting Testosterone Therapy for Hypogonadism in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0034) Aveed's Impact on Metabolic Health in American Men with Hypogonadism: Benefits and Considerations [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0035) Aveed: Enhancing Life for Diabetic Men with Low Testosterone [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0036) Aveed's Impact on Skin Health: Benefits and Risks for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Aveed: Enhancing Immune Function in American Men with Testosterone Deficiency [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Aveed: Enhancing Cardiovascular Fitness in American Men with Testosterone Therapy [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0039) Aveed Therapy Enhances Sleep Quality in Men with Low Testosterone: Clinical Insights [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0040) Aveed Therapy: Importance of Regular Blood Tests for Monitoring and Safety [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0041) Aveed Therapy: Understanding Its Impact on Hair Loss in Men with Low Testosterone [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) Aveed: Long-Acting Testosterone Therapy for Men with Heart Disease and Low Testosterone [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Aveed: Revolutionizing Testosterone Therapy with Long-Acting Injections for Hypogonadism [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Aveed: Managing Hypogonadism and Chronic Pain in American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0045) Aveed: Revolutionizing Hypogonadism Treatment for American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0046) Aveed: Enhancing Post-Surgical Recovery with Long-Acting Testosterone Therapy [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0047) Aveed's Impact on Blood Pressure in Hypogonadism Treatment: Monitoring and Management [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) Aveed: Testosterone Therapy and Liver Health Monitoring for American Men [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0049) Aveed's Impact on Cholesterol: Monitoring and Management for American Men on TRT [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0050) Aveed: Enhancing Mental Clarity in American Men with Low Testosterone [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0051) Aveed: Enhancing Athletic Performance in American Men with Testosterone Therapy [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0052) Maximizing Aveed Therapy Benefits: Diet, Exercise, Sleep, and Lifestyle for American Men [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0053) Aveed: Revolutionizing Low Testosterone Treatment in American Men [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0054) Aveed: Enhancing Digestive Health in American Men Through Testosterone Therapy [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0055) Aveed for Hypogonadism: Benefits and Kidney Function Risks in American Men [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0056) Aveed's Impact on Vision: Monitoring and Managing Side Effects in American Men [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0057) Enhancing Mental Health Support for Men on Aveed Therapy: A Multifaceted Approach [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0058) Aveed: Enhancing Life for American Men with Low Testosterone and Respiratory Issues [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0059) Aveed: Testosterone Therapy's Potential in Enhancing Hearing in American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0060) Aveed: Revolutionizing Low Testosterone Treatment for American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0061) Aveed: Revolutionizing Hypogonadism Treatment for American Men's Health [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0062) Aveed: Revolutionizing Testosterone Therapy for American Men with Hypogonadism [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0063) Aveed: Effective Long-Acting Testosterone for Men with Neurological Disorders [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0064) Aveed Boosts Skin Elasticity in American Men with Low Testosterone: Benefits and Risks [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0065) Aveed: Enhancing Dental Health in American Men Through Testosterone Therapy [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0066) Aveed Therapy: Enhancing Joint Health in American Men with Hypogonadism [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0067) Aveed: Enhancing Nail Health in American Men Through Testosterone Therapy [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0068) Aveed Therapy: Importance of Regular Check-ups for Safe Treatment in American Men [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0069) Aveed: A Breakthrough in Treating Low Testosterone in American Men [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0070) Aveed: Testosterone Therapy's Role in Managing Hair Loss in American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0071) Aveed Therapy: Importance of Hormone Level Monitoring for American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0072) Aveed's Impact on Eye Health in American Men with Hypogonadism: Benefits and Risks [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0073) Aveed's Impact on Muscle Recovery in American Men with Low Testosterone [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0074) Aveed: Enhancing Bone Density in American Men with Hypogonadism [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0075) Aveed: Revolutionizing Low Testosterone Treatment with Less Frequent Dosing [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0076) Aveed: A Vital Solution for American Men with Autoimmune Diseases and Low Testosterone [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0077) Aveed: Revolutionizing Testosterone Therapy for American Men with Low T [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0078) Aveed: Enhancing Longevity in American Men with Hypogonadism [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0079) Aveed: Long-Acting Testosterone Therapy for American Males with Hypogonadism [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0080) Aveed: Long-Acting Testosterone Therapy for American Men with Hypogonadism [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
Word Count: 35