Introduction
In the high-pressure landscape of contemporary American society, where professional demands often eclipse personal fulfillment, a growing epidemic of low libido—clinically termed hypoactive sexual desire disorder (HSDD)—is afflicting males across demographics. Affecting an estimated 8-10% of U.S. men aged 18-59, according to data from the National Health and Nutrition Examination Survey (NHANES), this condition manifests as persistent diminished interest in sexual activity, profoundly impacting relationships, mental health, and overall quality of life. This article delves into the intricate interplay between work-life balance and sexual health, elucidating how chronic occupational stressors precipitate endocrine disruptions, fatigue, and relational discord, ultimately eroding libido. By examining epidemiological trends, pathophysiological mechanisms, and evidence-based interventions, we aim to empower American males with actionable insights for reclaiming vitality.
Defining Work-Life Imbalance and Its Prevalence
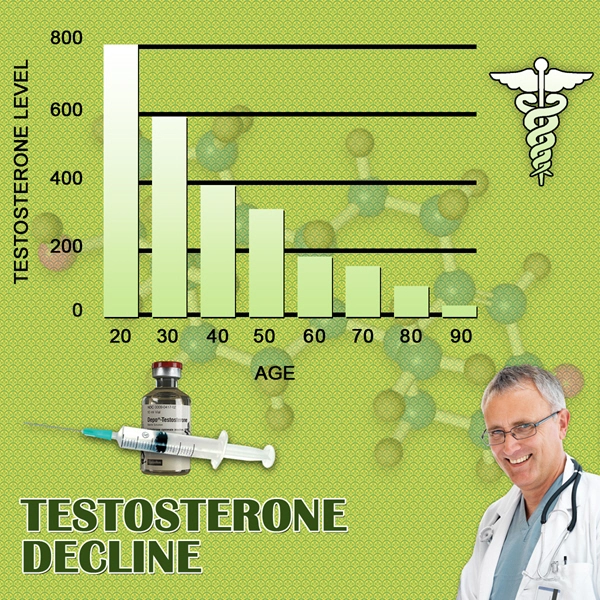
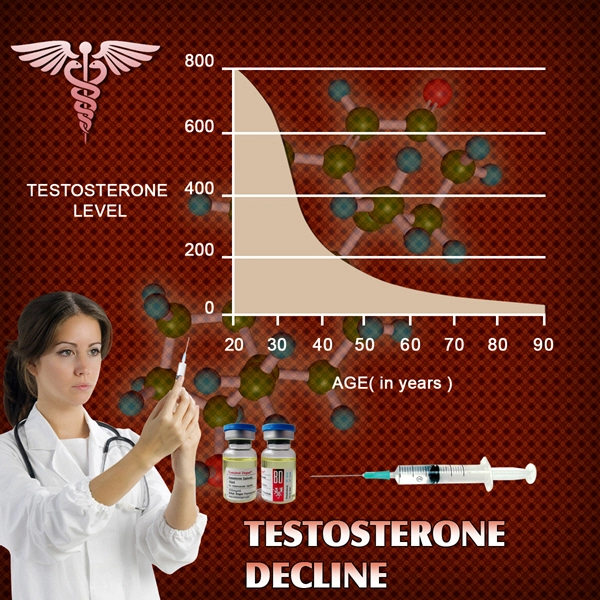
Work-life imbalance, characterized by excessive occupational commitments encroaching upon familial, recreational, and restorative activities, is rampant among American males. The Bureau of Labor Statistics reports that full-time male workers average 41.5 hours weekly, with over 20% exceeding 50 hours, particularly in sectors like finance, technology, and healthcare. This disequilibrium fosters a pernicious cycle: prolonged exposure to job-related stressors elevates cortisol levels, suppressing hypothalamic-pituitary-gonadal (HPG) axis function and diminishing testosterone bioavailability—key drivers of libido. Longitudinal studies, such as the Massachusetts Male Aging Study, corroborate this, revealing a 15-20% higher incidence of HSDD in men reporting poor work-life integration compared to balanced cohorts.
Chronic Stress: The Endocrine Saboteur
At the physiological core, chronic stress from work-life disequilibrium activates the hypothalamic-pituitary-adrenal (HPA) axis, culminating in hypercortisolemia. Elevated cortisol antagonizes testosterone synthesis in Leydig cells, reducing free androgen indices by up to 25%, as evidenced by randomized controlled trials in *The Journal of Clinical Endocrinology & Metabolism*. American males, navigating competitive corporate cultures and economic precarity—exacerbated by stagnant wages and gig economy pressures—experience amplified sympathetic nervous system dominance, manifesting as erectile dysfunction precursors and anhedonic sexual responses. Neuroimaging data further implicate prefrontal cortex hypoactivation, impairing reward processing essential for sexual arousal.
Disrupted Sleep and Circadian Rhythms
Extended work hours invariably compromise sleep hygiene, with 35% of U.S. male professionals reporting fewer than 6 hours nightly per the Centers for Disease Control and Prevention (CDC). Sleep fragmentation disrupts melatonin-testosterone pulsatility, yielding diurnal nadir levels akin to andropause. A meta-analysis in *Sleep Medicine Reviews* links insomnia to a 1.5-fold HSDD risk, as REM deprivation curtails erectile tissue oxygenation and dopamine surges critical for libido. For American fathers juggling 9-to-5 grinds with childcare, this chronobiological insult compounds, fostering fatigue-induced sexual aversion.
Psychosocial Ramifications on Intimate Relationships
Beyond biology, work-life imbalance erodes relational intimacy, a libido cornerstone. The American Psychological Association notes that 75% of men cite work stress as a primary marital discord factor, precipitating emotional distancing and reduced coital frequency. Attachment theory posits that perceived partner unavailability—stemming from exhaustion—triggers avoidance patterns, diminishing oxytocin-mediated bonding. Surveys from the Kinsey Institute reveal that men with suboptimal work-life balance report 40% lower sexual satisfaction scores, underscoring how professional burnout transmutes into bedroom barrenness.
Evidence-Based Interventions for Restoration
Reversing this trajectory demands multifaceted strategies. Cognitive-behavioral stress management (CBSM) programs, validated in NIH-funded trials, attenuate cortisol by 30% and boost testosterone within 12 weeks. Prioritizing 7-9 hours of sleep via circadian entrainment—e.g., blue-light mitigation—restores HPG integrity. Workplace advocacy for flexible scheduling, as piloted in Scandinavian models adapted for U.S. firms, yields 22% libido improvements per Harvard Business Review analyses. Nutraceuticals like ashwagandha (600mg daily) and phosphodiesterase-5 inhibitors, alongside aerobic exercise (150 minutes weekly), synergistically enhance vascular endothelial function and androgen receptor sensitivity. Routine testosterone assays and urological consultations are prudent for persistent cases.
Conclusion: A Call to Rebalance
The nexus of work-life imbalance and low libido in American males represents a modifiable public health imperative. By mitigating HPA hyperactivity, optimizing sleep architecture, and nurturing psychosocial bonds, men can reclaim sexual vitality. Policymakers must champion initiatives like paid family leave expansions under the Family and Medical Leave Act to foster systemic equilibrium. Ultimately, prioritizing holistic well-being over unchecked ambition promises not only enhanced eroticism but a fuller, more resilient life.
(Word count: 672)
Contact Us Today For A Free Consultation

- 0001) Physical Causes of Low Libido in American Males: Hormones, Illnesses, and Lifestyle [Last Updated On: February 20th, 2025] [Originally Added On: February 20th, 2025]
- 0002) Unraveling the Link Between Anxiety and Diminished Sexual Desire in American Men [Last Updated On: March 1st, 2025] [Originally Added On: March 1st, 2025]
- 0003) Revitalizing Desire: Strategies for Overcoming Low Libido in Long-term Relationships Among American Males [Last Updated On: March 1st, 2025] [Originally Added On: March 1st, 2025]
- 0004) Decoding Medical Science: A Comprehensive Approach To Low Libido Issues [Last Updated On: March 2nd, 2025] [Originally Added On: March 2nd, 2025]
- 0005) Comprehensive Overview of Male Libido Issues: Causes, Treatments, and Lifestyle Interventions [Last Updated On: March 3rd, 2025] [Originally Added On: March 3rd, 2025]
- 0006) Comprehensive Guide to Understanding and Managing Low Libido in Men [Last Updated On: March 4th, 2025] [Originally Added On: March 4th, 2025]
- 0007) Exploring Hormonal Influences on Male Libido: Testosterone, Thyroid, and Prolactin [Last Updated On: March 5th, 2025] [Originally Added On: March 5th, 2025]
- 0008) Understanding and Managing Low Libido in American Men: Causes and Treatments [Last Updated On: March 6th, 2025] [Originally Added On: March 6th, 2025]
- 0009) Understanding Post-Menopausal Libido: Hormonal, Physical, and Emotional Factors Impacting Sexual Desire [Last Updated On: March 7th, 2025] [Originally Added On: March 7th, 2025]
- 0010) Understanding Low Libido in Men: Causes, Impacts, and Effective Treatment Strategies [Last Updated On: March 8th, 2025] [Originally Added On: March 8th, 2025]
- 0011) Comprehensive Guide to Understanding and Managing Low Libido in Men: Psychological Perspectives and Solutions [Last Updated On: March 9th, 2025] [Originally Added On: March 9th, 2025]
- 0012) Navigating the Impact of Chronic Diseases on Male Libido: A Comprehensive Medical Insight [Last Updated On: March 14th, 2025] [Originally Added On: March 12th, 2025]
- 0013) Revitalizing Intimacy: Exploring Medical Therapies for Low Libido in Postpartum American Women [Last Updated On: March 13th, 2025] [Originally Added On: March 13th, 2025]
- 0014) Revitalizing Desire: Cutting-Edge Medical Treatments for Low Libido in American Males [Last Updated On: March 15th, 2025] [Originally Added On: March 15th, 2025]
- 0015) Psychological Causes of Low Libido in American Men: Stress, Depression, and More [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0016) Low Libido in American Males: Health Risks and the Importance of Seeking Help [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0017) Understanding Low Libido in American Males: Causes, Diagnosis, and Treatment Options [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0018) Medication-Induced Low Libido in American Males: Causes and Management Strategies [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0019) Understanding and Treating Low Libido in Men: Causes and Comprehensive Solutions [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0020) Diabetes and Male Libido: Understanding and Managing Low Sexual Desire [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0021) Chronic Illness Impact on Male Libido: Physiological, Psychological, and Management Strategies [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0022) Medications Impacting Male Libido: Insights and Management Strategies for American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0023) Natural Supplements for Low Libido in Men: Efficacy, Safety, and Holistic Approaches [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0024) Low Libido and Depression in American Males: Understanding and Treating the Connection [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0025) Advancements in Treating Low Libido in American Males: A Comprehensive Approach [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0026) Hyperthyroidism's Impact on Libido in American Males: Hormonal and Psychological Effects [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0027) Understanding Low Libido in Women Over 50: Insights for American Males [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0028) Understanding and Managing Low Libido in American Males: Causes, Diagnosis, and Treatment [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0029) Understanding and Addressing Low Libido in American Males: Causes, Diagnosis, and Treatment [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0030) Post-Pregnancy Low Libido in American Males: Causes and Solutions [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0031) Low Libido in American Males During Partner's Lactation: Causes and Solutions [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0032) Managing Low Libido in Male Surgical Patients: Causes, Impacts, and Strategies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0033) Understanding and Treating Low Libido in American Males: Causes and Solutions [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0034) Postpartum Libido in Men: Medical Tips and Strategies for Enhancement [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0035) Understanding and Addressing Low Libido in American Men: A Comprehensive Approach [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0036) Alcohol's Impact on Male Libido: Physiological Effects and Management Strategies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0037) Revitalizing Male Sexual Desire: Understanding and Treating Low Libido Holistically [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0038) Understanding and Addressing Low Libido in American Males: Causes, Impacts, and Solutions [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0039) Understanding and Addressing Low Libido in American Men: Medical and Lifestyle Approaches [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0040) Effective Interventions for Low Libido in American Men: A Comprehensive Guide [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0041) Revitalizing Sexual Desire in Middle-Aged Men: A Holistic Approach [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0042) Low Libido in American Women: Causes, Impacts, and Multifaceted Treatment Approaches [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0043) Exploring Risks and Side Effects of Low Libido Treatments in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0044) Post-Surgical Libido Recovery: Medical Tips for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0045) Understanding Low Libido in Men: Causes, Impacts, and Holistic Solutions [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0046) Understanding and Addressing Low Libido in American Men: Causes and Solutions [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0047) Chronic Pain and Low Libido: Understanding the Medical Connection in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0048) Managing Low Libido in Male Athletes: Hormonal, Nutritional, and Psychological Strategies [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0049) Understanding and Overcoming Low Libido in American Males: A Comprehensive Guide [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0050) Sudden Low Libido in American Males: Medical, Psychological, and Lifestyle Factors [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0051) Addressing Low Libido in American Males: Psychological, Physiological, and Lifestyle Factors [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0052) Understanding and Treating Low Libido in American Men: A Holistic Approach [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0053) Strategies to Boost Low Libido in American Males: Medical and Lifestyle Approaches [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0054) Low Libido in American Men: Causes, Treatments, and Lifestyle Impacts [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0055) Exploring Low Libido in Men: Causes, Treatments, and Personalized Approaches [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0056) Exploring Medical Patterns of Low Libido in Young American Males: Causes and Treatments [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0057) Exploring the Link Between Low Libido and Weight Gain in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0058) Hypertension's Impact on Libido in American Men: Causes and Management Strategies [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0059) Low Libido in American Males: Causes, Risks, and Medical Importance [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0060) Chronic Low Libido in American Males: Medical Signs and Management Strategies [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0061) Age-Related Low Libido in Men: Causes, Treatments, and Future Innovations [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0062) Low Libido and Unhappiness in American Men: Medical Insights and Interventions [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0063) Lifestyle Changes to Boost Libido in American Males: A Medical Perspective [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0064) Managing Low Libido in American Males Post-Chemotherapy: Medical and Lifestyle Approaches [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0065) Revitalizing Sexual Health: Understanding and Overcoming Low Libido in American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0066) Understanding and Treating Low Libido in Men: A Holistic Approach [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0067) Exploring Medical Causes and Solutions for Low Libido in American Men [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0068) Antidepressants and Low Libido in American Males: Causes, Impacts, and Management Strategies [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0069) Understanding Low Libido in Women: Medical Insights for American Males [Last Updated On: April 4th, 2025] [Originally Added On: April 4th, 2025]
- 0070) Exploring Causes and Solutions for Low Libido in American Men [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0071) Understanding and Addressing Low Libido in American Men: Medical Insights and Solutions [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0072) Understanding and Addressing Low Libido in American Males: Causes, Impacts, and Solutions [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0073) Medical Procedures Impacting Libido in American Men: Causes and Management Strategies [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0074) Medical Factors Impacting Low Libido in Women Under 40: Insights and Solutions [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0075) Addressing Low Libido in Men: Causes, Diagnosis, and Multifaceted Treatment Approaches [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0076) Medical Causes and Management of Low Libido in American Men [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0077) Medical Causes and Treatments for Low Libido in American Men [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0078) Managing Low Libido in American Males: Causes, Impacts, and Holistic Approaches [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0079) Understanding and Addressing Low Libido in American Males: A Holistic Approach [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0080) Understanding and Treating Low Libido in Men: Causes and Solutions [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
Word Count: 668