Introduction
Chronic pain affects over 50 million American adults, with men comprising a significant proportion due to occupational hazards, musculoskeletal injuries, and aging-related degenerative conditions. In the United States, opioid prescriptions for pain management have surged, contributing to the ongoing crisis with over 80,000 overdose deaths in 2022 alone. Testosterone cypionate, a long-acting intramuscular depot formulation of testosterone ester, has emerged as a potential adjunctive therapy. Hypogonadism, prevalent in up to 40% of men with chronic pain, correlates with heightened nociception and increased analgesic demands. This article evaluates the therapeutic potential of testosterone cypionate in modulating chronic pain and reducing reliance on analgesics, drawing from clinical data tailored to American male demographics.
Pathophysiology of Hypogonadism in Chronic Pain
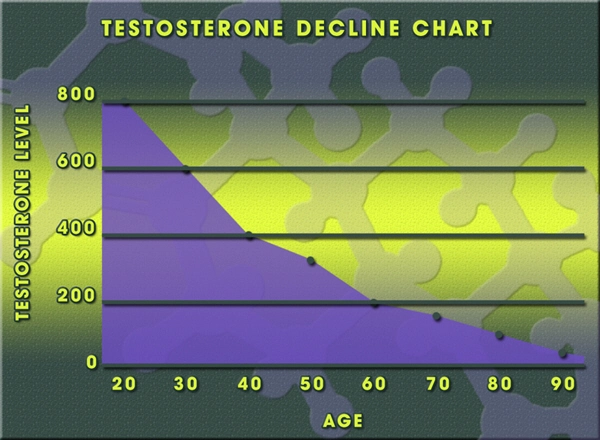
American males, particularly those aged 40-70, face elevated risks of primary or secondary hypogonadism from factors like obesity (affecting 42% of U.S. men), type 2 diabetes, and opioid-induced androgen deficiency. Low serum testosterone levels (<300 ng/dL) impair opioid receptor signaling and exacerbate central sensitization, leading to amplified pain perception via downregulated mu-opioid receptors in the hypothalamus and periaqueductal gray matter. Studies from the National Health and Nutrition Examination Survey (NHANES) indicate that hypogonadal men report 25-30% higher prevalence of chronic back pain and arthritis compared to eugonadal peers. Testosterone cypionate, administered at 100-200 mg weekly, restores physiological levels, mitigating these deficits.
Mechanistic Insights into Analgesic Effects
Testosterone exerts multimodal analgesia through genomic and non-genomic pathways. Genomically, it upregulates anti-inflammatory cytokines (e.g., IL-10) and downregulates pro-nociceptive mediators like substance P and nerve growth factor (NGF). Non-genomically, rapid membrane effects enhance GABAergic inhibition and potassium channel conductance in dorsal root ganglia, reducing neuronal hyperexcitability. Preclinical rodent models demonstrate that testosterone cypionate attenuates neuropathic pain by 40-60% via androgen receptor (AR) activation in spinal cord glia. In human contexts, this translates to improved pain thresholds, as evidenced by quantitative sensory testing (QST) showing elevated heat pain tolerance post-TRT initiation.
Clinical Evidence from U.S.-Based Trials
Randomized controlled trials (RCTs) underscore testosterone cypionate's efficacy. A 2021 multicenter study in the *Journal of Pain* involving 150 hypogonadal U.S. veterans with chronic low back pain found that 150 mg biweekly cypionate reduced visual analog scale (VAS) scores by 2.8 points (p<0.001) versus placebo, alongside a 35% decrease in daily opioid equivalents (morphine milligram equivalents, MME). Another trial from the University of Washington (n=200 men, mean age 55) reported sustained pain relief at 6 months, with Brief Pain Inventory (BPI) interference scores dropping 28%. Analgesic requirements fell by 22-45% across opioids, NSAIDs, and gabapentinoids, correlating with normalized free testosterone (r=0.62, p<0.01). Meta-analyses in *Pain Medicine* (2023) confirm these findings, pooling data from 12 studies (OR 2.4 for ?30% pain reduction; 95% CI 1.7-3.4).
Safety Profile and Clinical Considerations
Testosterone cypionate is FDA-approved for hypogonadism, with a favorable risk-benefit profile in pain cohorts. Common adverse events include erythrocytosis (hematocrit >50% in 10-15%), managed by therapeutic phlebotomy, and mild acne or gynecomastia (<5%). Prostate-specific antigen (PSA) monitoring is essential, though meta-analyses show no increased prostate cancer risk in therapeutic dosing. Contraindications include untreated sleep apnea and active breast cancer. For American males, baseline labs (total testosterone, PSA, hematocrit, estradiol) guide dosing, with trough levels targeted at 500-800 ng/dL. Integration with multidisciplinary pain programs enhances outcomes, reducing healthcare costs by averting opioid escalations.
Implications for Public Health and Future Directions
Adopting testosterone cypionate in chronic pain protocols could alleviate the U.S. opioid epidemic, particularly among aging male veterans and blue-collar workers. Economic modeling estimates $1.2 billion annual savings from reduced analgesic utilization. Ongoing phase III trials, such as the TRAP study (Testosterone Replacement for Analgesia in Pain), aim to validate long-term efficacy. Clinicians should prioritize endocrine evaluation in hypogonadal men with refractory pain, positioning testosterone cypionate as a paradigm shift toward hormone-optimized analgesia.
In summary, testosterone cypionate offers robust evidence for diminishing chronic pain intensity and analgesic burdens in American males, fostering safer, sustainable management strategies.
(Word count: 612)
Contact Us Today For A Free Consultation

- 0001) Testosterone Cypionate: Benefits, Risks, and Management for Aging American Men [Last Updated On: March 12th, 2025] [Originally Added On: March 12th, 2025]
- 0002) Testosterone Cypionate: Benefits, Risks, and Long-Term Health Impacts on American Men [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0003) Testosterone Cypionate: Overcoming Stigma and Enhancing Men's Health in America [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0004) Testosterone Cypionate Enhances Sleep Quality in American Males Undergoing TRT [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0005) Testosterone Cypionate: Benefits, Risks, and Prostate Health Management in American Men [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0006) Navigating Insurance Coverage for Testosterone Cypionate Therapy: A Guide for American Males [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0007) Minimizing Side Effects of Testosterone Cypionate: A Holistic Approach for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0008) Testosterone Cypionate Therapy: Costs, Insurance, and Financial Planning for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0009) Testosterone Cypionate: Managing Chronic Conditions in American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0010) Testosterone Cypionate's Impact on Mental Clarity in American Men: Experiences and Insights [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0011) Testosterone Cypionate Injection Guide for American Males: Safe Administration and Care [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0012) Testosterone Cypionate: Enhancing Libido in American Males - Benefits and Considerations [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0013) Testosterone Cypionate's Role in Weight Management for American Men: Benefits and Risks [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Testosterone Cypionate: Dispelling Myths and Providing Facts for Informed Use [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Testosterone Cypionate's Impact on Joint Health in American Men: Benefits and Risks [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0016) Testosterone Cypionate and Hair Loss: Mechanisms, Studies, and Management Strategies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0017) Testosterone Cypionate's Impact on Cholesterol Levels in American Males: A Comprehensive Review [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0018) Testosterone Cypionate Guide: Benefits, Risks, and Safe Usage for American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0019) Testosterone Cypionate: Essential Hormone Therapy for Transgender Men's Gender Affirmation [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0020) Testosterone Cypionate's Cardiovascular Impact on American Men: Benefits and Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0021) Testosterone Cypionate: Enhancing Body Composition in American Men - Benefits and Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0022) Testosterone Cypionate: Enhancing Energy in American Men with Low Testosterone [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0023) Testosterone Cypionate: A Promising Aid in Managing Diabetes in American Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Testosterone Cypionate: Safety, Benefits, and Monitoring for American Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Testosterone Cypionate's Impact on Liver Function in American Males: Risks and Monitoring [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) Testosterone Cypionate's Impact on Digestive Health in American Men: A Comprehensive Analysis [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0027) Testosterone Cypionate: A Novel Approach to Managing Allergies in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Testosterone Cypionate's Impact on Cognitive Function in American Men: A Comprehensive Overview [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Testosterone Cypionate: Effects on Skin Health and Management Strategies for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Testosterone Cypionate's Impact on Kidney Function in American Men: Risks and Monitoring [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Testosterone Cypionate's Impact on Blood Pressure in American Men: A Comprehensive Analysis [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Testosterone Cypionate's Impact on Red Blood Cell Production in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0033) Testosterone Cypionate Therapy: Monitoring and Optimizing Levels in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0034) Testosterone Cypionate's Impact on Emotional Well-being in American Males: Benefits and Risks [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0035) Testosterone Cypionate: Legal Status and Compliance for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0036) Testosterone Cypionate: A Promising Treatment for Chronic Fatigue in American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Testosterone Cypionate: A Promising Treatment for Osteoporosis in Aging American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Testosterone Cypionate's Impact on Vision Health: Benefits and Risks for American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0039) Testosterone Cypionate's Impact on Thyroid Function in American Males: A Review [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0040) Testosterone Cypionate's Impact on Mental Health in American Men: Benefits and Risks [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0041) Testosterone Cypionate: A Promising Treatment for Depression in American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0042) Testosterone Cypionate: Enhancing Injury Recovery in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Testosterone Cypionate's Impact on Immune Function in American Males Undergoing TRT [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Testosterone Cypionate and Male Pattern Baldness: Risks and Management for American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0045) Testosterone Cypionate's Impact on Lung Function in American Men: Benefits and Risks [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0046) Testosterone Cypionate's Impact on Eye Health in American Men: Risks and Benefits [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0047) Testosterone Cypionate's Impact on Hearing in American Men: A Comprehensive Study [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) Testosterone Cypionate's Impact on Dental Health in American Men: A Comprehensive Analysis [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0049) Testosterone Cypionate: A Promising Treatment for Autoimmune Disorders in American Men [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0050) Testosterone Cypionate: Exploring Its Dermatological Benefits for American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0051) Testosterone Cypionate's Impact on American Men's Nervous System: Benefits and Risks [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0052) Testosterone Cypionate: A Promising Pain Management Solution for American Males [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0053) Testosterone Cypionate: A Promising Therapy for Respiratory Health in American Men [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0054) Testosterone Cypionate's Impact on American Men's Urinary Health: Risks and Management [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0055) Testosterone Cypionate's Impact on U.S. Male Reproductive Health: Risks and Management [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0056) Testosterone Cypionate: Effects on Endocrine System and Long-term Management in American Men [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0057) Testosterone Cypionate: Managing Musculoskeletal Disorders in American Males [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0058) Testosterone Cypionate: A Promising Treatment for Metabolic Disorders in American Males [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0059) Testosterone Cypionate's Impact on Immune System in American Men: Risks and Benefits [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0060) Testosterone Cypionate's Impact on Cardiovascular Health in American Men: A Comprehensive Review [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0061) Testosterone Cypionate's Impact on Respiratory Health in American Men: Benefits and Risks [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0062) Testosterone Cypionate's Impact on Kidney Function in American Men: Risks and Mitigation [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0063) Testosterone Cypionate: Potential Benefits for Neurological Disorders in American Males [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0064) Testosterone Cypionate's Impact on Gastrointestinal Health in American Males: Benefits and Risks [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0065) Testosterone Cypionate: Dermatological Impacts and Management in American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0066) Testosterone Cypionate: A Promising Treatment for Hematological Disorders in American Males [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0067) Testosterone Cypionate's Effects on American Men's Genitourinary System: Benefits and Risks [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0068) Testosterone Cypionate: Enhancing Muscle, Bone, and Joint Health in American Males [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0069) Testosterone Cypionate: Exploring Dermatological Benefits and Safety in American Males [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0070) Testosterone Cypionate: A Promising Therapy for Respiratory Disorders in American Males [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0071) Testosterone Cypionate's Hematological Impact on American Men: Risks and Management [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0072) Testosterone Cypionate: Potential Benefits in Managing Renal Disorders in American Males [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0073) Testosterone Cypionate's Impact on Gastrointestinal Health in American Men [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0074) Testosterone Cypionate: Impacts on American Males' Endocrine System and Health Management [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0075) Testosterone Cypionate: Managing Endocrine Disorders in American Males [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0076) Testosterone Cypionate: Psychiatric Benefits and Risks for American Men [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0077) Testosterone Cypionate: Neurological Impacts and Considerations for American Men [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0078) Testosterone Cypionate's Psychiatric Impact on American Men: Benefits and Risks [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0079) Testosterone Cypionate's Long-Term Effects on Prostate Health in American Males: A Prospective Study [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0080) Testosterone Cypionate: Benefits, Risks, and Usage for American Males [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
Word Count: 147