Low-T and Your Health
Video Link: https://vimeo.com/293590145
Video Download: Click Here To Download Video
Video Stream: Click Here To Stream Video
How Does the Body Produce Testosterone?
The production of Testosterone is the result of a cascade of hormone signals, with a cycle beginning at the hypothalamus. When the hypothalamus receives  the signal to produce Testosterone, it releases a hormone known as Gonadotropin-Releasing Hormone, usually referred to in scientific literature as GnRH.
the signal to produce Testosterone, it releases a hormone known as Gonadotropin-Releasing Hormone, usually referred to in scientific literature as GnRH.
In both sexes, GnRH travels through the Hypophyseal Portal System from the Hypothalamus to the Pituitary, where it stimulates the production of two important hormones: Luteinizing Hormone (LH) and Follicle Stimulating Hormone (FSH).
From here, the sex hormone cycle differs for both sexes. In women, Follicle Stimulating Hormone prepares for the release of an egg by stimulating the production of fluid pouches known as follicles which store the developed egg in preparation for fertilization.
Luteinizing Hormone, on the other hand, encourages ovulation. In men, on the other hand, the two hormones are associated with the production of Testosterone and Sperm.
Luteinizing Hormone travels to the testes, where it activates cells known at Leydig Cells that are responsible for the production of Testosterone. Follicle-Stimulating Hormone travels to Sertoli Cells in the Testes, which encourage the production of sperm.
Some Testosterone that is produced by the testes is naturally converted into Estrogen by various tissues, including adipose fat tissue.
Estrogen Levels in the male bloodstream are monitored by the Hypothalamus, and Estrogen activates receptors in the Hypothalamus which modulate the release of upstream Testosterone Precursors, creating a cycle that is designed to maintain balanced Testosterone Production.
When this hormone balance is disrupted, it contributes to Andropause.
What Causes Low-T?
There are three categories of Testosterone Deficiency, dependent upon the source of the deficiency: Primary, Secondary, and Tertiary Low-T.
Primary Testosterone Deficiency is the result of a malfunction of the testes which prevents Testosterone from being adequately produced to meet the needs of the  body. This is a rare form of natural Low-T and is generally the result of damage to the testes resulting from trauma, injury, surgery, cancer, or other illnesses.
body. This is a rare form of natural Low-T and is generally the result of damage to the testes resulting from trauma, injury, surgery, cancer, or other illnesses.
Secondary Testosterone Deficiency is the result of inadequacies within the Pituitary Gland which prevent the body from producing the Testosterone that it needs.
In general, Secondary Testosterone Deficiency is also quite rare. The pituitary generally retains its ability to produce the various hormones that are associated with the organ, and the issue tends to be that the organ does not receive the required stimulation to produce such hormones.
Tertiary Testosterone Deficiency is caused by changes in the hypothalamic activity which contribute to the suppressed production of Testosterone.
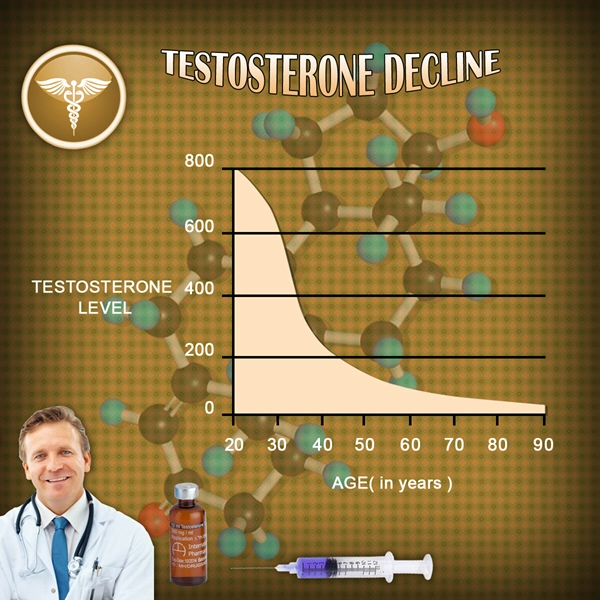
This is generally the root cause of Andropause, the age-related decline in Testosterone Production which leads to symptoms such as Loss of Sex Drive, Suppressed Libido, and unwanted changes in body composition.
How is Low-T Treated?
Depending on the form of Testosterone Treatment, there are a number of forms of Testosterone Therapy available for patients suffering from Low-T.
Primary Testosterone Deficiency Treatment
For patients suffering from Primary Testosterone Deficiency, the only form of treatment is Bio-Identical Testosterone Therapy, but there are a variety of ways to deliver the therapy effectively, including Testosterone Patches, Creams, Injections, and Implants.
These products provide a regular supply of Testosterone to sustain normal male health and physiology.
Secondary Testosterone Deficiency Treatment
For Secondary Testosterone Deficiency resulting from Pituitary Insufficiency, the range of options is slightly larger. All forms of Bio-Identical Low-T Therapy are effective, and these patients also have the opportunity to use HCG Therapy. HCG is a functional analog of Luteinizing Hormone.
It is a naturally occurring hormone that is produced by women, and, when used as a medical treatment in men, mimics the actions of Luteinizing Hormone in the male body, stimulating the production of testosterone by the Leydig Cells.
Tertiary Testosterone Deficiency Treatment
Low-T caused by upstream issues with the hypothalamus has the widest range of options available.
Both Testosterone Therapy and HCG can benefit patients with Tertiary Low-T, as well as hormones that alter the signaling patterns of the Hypothalamus.
For example, Clomiphene Citrate is a Selective Estrogen Receptor Modulator that suppresses the negative feedback mechanism associated with Estrogen which inhibits the production of Testosterone, one of the leading contributors to Andropause.
By reducing the influence of Estrogen on the Hypothalamus, it is possible to increase the production of Testosterone to more naturally healthy levels.
Combination Testosterone Therapy
Testosterone Therapy is the most popular treatment for Low-T, and it is often combined with other forms of treatment in order to maximize the success of therapy.
These secondary treatments are combined with Testosterone Therapy in order to mitigate the side-effects that are sometimes associated with treatment.
Testosterone with HCG
Human Chorionic Gonadotropin can be used on its own as a means to enhance Testosterone Levels, and it can also be combined with Testosterone Therapy in order to sustain fertility and normal testicular function and appearance during therapy.
When Bio-Identical Testosterone is prescribed on its own, it provides all of its great benefits but has two unavoidable side effects: Suppressed Fertility and  Testicular Shrinkage. By adding Bio-Identical HCG to normal Testosterone Treatment, it is possible to eliminate these two side effects.
Testicular Shrinkage. By adding Bio-Identical HCG to normal Testosterone Treatment, it is possible to eliminate these two side effects.
Testosterone with Estrogen Blockers
As we mentioned earlier, the presence of Testosterone in the bloodstream encourages an elevation in Estrogen production due to the conversion of Testosterone into Estrogen.
If the body is producing too much Estrogen, this can lead to symptoms such as gynecomastia and edema which can be problematic.
By combining Estrogen Blockers with Low-T Therapy, it is possible to mitigate these symptoms of elevated Estrogen Levels in the bloodstream, improving how the body takes to the treatment.
Estrogen Blockers also help preserve fertility and prevent testicular shrinkage like HCG.
These Estrogen Blockers can also be used as a substitute for Testosterone at sufficient doses for some patients, especially those that are interested in having children while simultaneously benefiting from enhanced Testosterone Levels.
Testosterone with Human Growth Hormone
Many patients simultaneously suffer from multiple forms of Hormone Deficiency simultaneously. Both HGH Deficiency and Testosterone Deficiency are Age-Associated conditions which share many symptoms with one another.
Many Hormone Clinics provide what is known as a Comprehensive Hormone Panel to provide the prescribing physician with a full set of health and hormone data that can accurately reveal a variety of hormone, health, and nutritional deficiencies.
HGH Restoration can be achieved through two primary mechanisms, Bio-Identical Human Growth Hormone Injections, and Sermorelin Acetate Injections.
Contact Us Today For A Free Consultation

- 0001) Adverse Effects of Testosterone Therapy in Adult Men: A Systematic Review and Meta-Analysis [Last Updated On: July 2nd, 2024] [Originally Added On: June 4th, 2010]
- 0002) Low Testosterone Levels, Foods That Increase Testosterone Levels wwwSelf-Improvement-Bible.com [Last Updated On: November 12th, 2023] [Originally Added On: May 30th, 2011]
- 0003) Low Testosterone in Men: The Next Big Thing in Medicine! - Abraham Morgentaler, MD [Last Updated On: May 7th, 2023] [Originally Added On: June 3rd, 2011]
- 0004) How To Determine Testosterone Levels By Looking At Your Ring Finger [Last Updated On: January 28th, 2026] [Originally Added On: June 30th, 2011]
- 0005) Prolab Horny Goat Weed Testosterone Booster Supplement Review [Last Updated On: November 23rd, 2023] [Originally Added On: July 19th, 2011]
- 0006) The Healthy Skeptic: Products make testosterone claims [Last Updated On: August 13th, 2024] [Originally Added On: September 11th, 2011]
- 0007) How To Naturally Increase Testosterone [Last Updated On: November 21st, 2023] [Originally Added On: September 28th, 2011]
- 0008) Testosterone Production - Video [Last Updated On: November 25th, 2024] [Originally Added On: November 20th, 2011]
- 0009) Testosterone makes us less cooperative and more egocentric, study finds [Last Updated On: January 23rd, 2018] [Originally Added On: February 1st, 2012]
- 0010) Testosterone makes us less cooperative and more egocentric [Last Updated On: January 24th, 2018] [Originally Added On: February 1st, 2012]
- 0011) Too much testosterone makes for bad decisions, tests show [Last Updated On: April 30th, 2025] [Originally Added On: February 1st, 2012]
- 0012) Today in Research: Testosterone's Negative Effects; Diet Soda Death [Last Updated On: January 2nd, 2018] [Originally Added On: February 2nd, 2012]
- 0013) Testosterone drives ego, trips cooperation [Last Updated On: December 25th, 2025] [Originally Added On: February 4th, 2012]
- 0014) FDA approves BioSante/Teva's testosterone gel [Last Updated On: April 28th, 2025] [Originally Added On: February 15th, 2012]
- 0015) 'Manly' Fingers Make For Strong Jawline in Young Boys [Last Updated On: December 14th, 2025] [Originally Added On: February 15th, 2012]
- 0016) Teva, BioSante Win U.S. Approval for Testosterone Therapy [Last Updated On: February 10th, 2026] [Originally Added On: February 15th, 2012]
- 0017) BioSante Gains on Approval of Testosterone Gel: Chicago Mover [Last Updated On: January 8th, 2018] [Originally Added On: February 16th, 2012]
- 0018) BioSante soars following drug approval from FDA [Last Updated On: December 26th, 2017] [Originally Added On: February 16th, 2012]
- 0019) Antibodies, Not Hard Bodies: The Real Reason Women Drool Over Brad Pitt [Last Updated On: December 24th, 2017] [Originally Added On: February 21st, 2012]
- 0020) Almark Publishing Releases Book From Mark Rosenberg, M.D. Revealing Natural Discoveries Associated With Low ... [Last Updated On: May 3rd, 2025] [Originally Added On: February 28th, 2012]
- 0021) Testosterone Replacement Clinic Comes to Kansas City with Potential to Help Thousands of Men [Last Updated On: May 2nd, 2025] [Originally Added On: March 1st, 2012]
- 0022) Study examines the relative roles of testosterone and its metabolite, dihydrotestosterone in men [Last Updated On: December 23rd, 2025] [Originally Added On: March 7th, 2012]
- 0023) The Role of 5{alpha}-Reductase Inhibition in Men Receiving Testosterone Replacement Therapy [Editorial] [Last Updated On: December 21st, 2017] [Originally Added On: March 7th, 2012]
- 0024) Effect of Testosterone Supplementation With and Without a Dual 5{alpha}-Reductase Inhibitor on Fat-Free Mass in Men ... [Last Updated On: January 3rd, 2018] [Originally Added On: March 7th, 2012]
- 0025) Why We Like Men Who Can Keep Their Cool [Last Updated On: December 30th, 2017] [Originally Added On: March 7th, 2012]
- 0026) Testosterone And Heart Health [Last Updated On: May 1st, 2025] [Originally Added On: March 10th, 2012]
- 0027) Your Life on Testosterone: Overly Sure of Yourself, Unwilling to Listen [Last Updated On: November 25th, 2018] [Originally Added On: March 15th, 2012]
- 0028) Mayo Clinic-TGen study role testosterone may play in triple negative breast cancer [Last Updated On: February 1st, 2026] [Originally Added On: March 23rd, 2012]
- 0029) A dose of testosterone might not cure what ails you [Last Updated On: January 23rd, 2018] [Originally Added On: March 25th, 2012]
- 0030) Green tea could aid athletes hide testosterone doping [Last Updated On: March 16th, 2026] [Originally Added On: March 25th, 2012]
- 0031) TGen Study Role Testosterone May Play in Triple Negative Breast Cancer [Last Updated On: January 19th, 2026] [Originally Added On: March 26th, 2012]
- 0032) Testosterone low, but responsive to competition, in Amazonian tribe [Last Updated On: January 23rd, 2018] [Originally Added On: March 28th, 2012]
- 0033) Competition-linked bursts of testosterone are fundamental aspect of human biology, study of Amazonian tribe suggests [Last Updated On: December 25th, 2017] [Originally Added On: March 28th, 2012]
- 0034) Playing football boosts testosterone levels by 30 percent! [Last Updated On: February 4th, 2024] [Originally Added On: March 28th, 2012]
- 0035) Testosterone low, but responsive to competition, in Amazonian tribe -- with slideshow [Last Updated On: February 3rd, 2026] [Originally Added On: March 28th, 2012]
- 0036) The benefits of testosterone pellet therapy [Last Updated On: January 24th, 2018] [Originally Added On: March 29th, 2012]
- 0037) Low testosterone levels cause health woes [Last Updated On: November 25th, 2018] [Originally Added On: March 30th, 2012]
- 0038) Heart Failure Patients Getting Relief from Testosterone Supplements [Last Updated On: May 5th, 2025] [Originally Added On: April 21st, 2012]
- 0039) Study Finds Fatherhood Suppresses Testosterone [Last Updated On: May 4th, 2025] [Originally Added On: May 3rd, 2012]
- 0040) Low testosterone levels could raise diabetes risk for men [Last Updated On: January 26th, 2018] [Originally Added On: May 5th, 2012]
- 0041) Why low testosterone may increase your risk of diabetes [Last Updated On: November 25th, 2024] [Originally Added On: May 5th, 2012]
- 0042) Diabetes link to low testosterone [Last Updated On: November 25th, 2024] [Originally Added On: May 5th, 2012]
- 0043) Testosterone Linked to Weight Loss in Obese Men [Last Updated On: January 2nd, 2018] [Originally Added On: May 11th, 2012]
- 0044) Testosterone may help weight loss [Last Updated On: November 25th, 2024] [Originally Added On: May 11th, 2012]
- 0045) Testosterone-fuelled infantile males might be a product of Mom's behaviour [Last Updated On: December 25th, 2017] [Originally Added On: May 11th, 2012]
- 0046) Testosterone-fueled infantile males might be a product of Mom's behavior [Last Updated On: January 6th, 2018] [Originally Added On: May 11th, 2012]
- 0047) Testosterone supplements may help obese men lose weight [Last Updated On: January 5th, 2018] [Originally Added On: May 11th, 2012]
- 0048) Testosterone supplements 'can help men lose their middle-aged spread' [Last Updated On: November 25th, 2024] [Originally Added On: May 12th, 2012]
- 0049) Some doctors question safety of testosterone replacement therapy [Last Updated On: January 20th, 2018] [Originally Added On: May 15th, 2012]
- 0050) Health Canada Approves New Testosterone Topical Solution for Men [Last Updated On: May 15th, 2025] [Originally Added On: May 15th, 2012]
- 0051) Environment trumps genes in testosterone levels, study finds [Last Updated On: May 8th, 2025] [Originally Added On: May 15th, 2012]
- 0052) Global Testosterone Replacement Therapy (TRT) Industry [Last Updated On: May 7th, 2025] [Originally Added On: May 21st, 2012]
- 0053) Testosterone Fuels Boom, Swindler Sows Panic: Top Business Books [Last Updated On: January 13th, 2018] [Originally Added On: June 2nd, 2012]
- 0054) Increase in testosterone drug use [Last Updated On: April 12th, 2018] [Originally Added On: June 4th, 2012]
- 0055) Testosterone Promotes Agression Automatically [Last Updated On: January 29th, 2018] [Originally Added On: June 9th, 2012]
- 0056) Testosterone shown to help sexually frustrated women [Last Updated On: January 27th, 2018] [Originally Added On: June 9th, 2012]
- 0057) Research and Markets: Testosterone Replacement Therapy (TRT) - Global Strategic Business Report [Last Updated On: December 23rd, 2017] [Originally Added On: June 12th, 2012]
- 0058) Proposed testosterone testing of some female olympians challenged by Stanford scientists [Last Updated On: January 30th, 2018] [Originally Added On: June 14th, 2012]
- 0059) Testosterone Makes Bosses Into Jerks, Says Paul Zak [Last Updated On: January 8th, 2018] [Originally Added On: June 14th, 2012]
- 0060) Testosterone Therapy: A Misguided Approach to Erectile Dysfunction (ED) [Last Updated On: May 10th, 2025] [Originally Added On: June 20th, 2012]
- 0061) New drugs, new ways to target androgens in prostate cancer therapy [Last Updated On: January 8th, 2018] [Originally Added On: June 20th, 2012]
- 0062) Long-term testosterone treatment for men results in reduced weight and waist size [Last Updated On: January 19th, 2018] [Originally Added On: June 23rd, 2012]
- 0063) Declining testosterone levels in men not part of normal aging, study finds [Last Updated On: December 27th, 2017] [Originally Added On: June 23rd, 2012]
- 0064) Low testosterone not normal part of aging [Last Updated On: December 22nd, 2017] [Originally Added On: June 25th, 2012]
- 0065) Testosterone Does Not Necessarily Wane With Age [Last Updated On: January 16th, 2026] [Originally Added On: June 25th, 2012]
- 0066) Overweight men can boost low testosterone levels by losing weight [Last Updated On: February 8th, 2026] [Originally Added On: June 25th, 2012]
- 0067) Testosterone-replacement therapy improves symptoms of metabolic syndrome [Last Updated On: January 14th, 2018] [Originally Added On: June 26th, 2012]
- 0068) Testosterone therapy takes off pounds [Last Updated On: February 14th, 2026] [Originally Added On: June 26th, 2012]
- 0069) Weight loss may boost men's testosterone [Last Updated On: May 9th, 2025] [Originally Added On: June 27th, 2012]
- 0070) Low Testosterone? Study finds age may not be to blame [Last Updated On: May 12th, 2025] [Originally Added On: July 1st, 2012]
- 0071) Do you have low testosterone? [Last Updated On: March 5th, 2026] [Originally Added On: July 8th, 2012]
- 0072) Wall Streeters Buying Testosterone for an Edge [Last Updated On: May 11th, 2025] [Originally Added On: July 12th, 2012]
- 0073) Beefy Wall Street Traders rub on testosterone [Last Updated On: February 20th, 2024] [Originally Added On: July 12th, 2012]
- 0074) Tale of two runners exposes flawed Olympic thinking [Last Updated On: December 23rd, 2024] [Originally Added On: July 19th, 2012]
- 0075) Genetic markers for testosterone and estrogen level regulation identified [Last Updated On: January 6th, 2018] [Originally Added On: July 20th, 2012]
- 0076) BUSM researchers identify genetic markers for testosterone, estrogen level regulation [Last Updated On: March 19th, 2026] [Originally Added On: July 20th, 2012]
- 0077) DRS. OZ AND ROIZEN: How to reap the benefits of normal testosterone levels [Last Updated On: December 23rd, 2024] [Originally Added On: July 21st, 2012]
- 0078) How Testosterone Drives History [Last Updated On: December 24th, 2024] [Originally Added On: July 22nd, 2012]
- 0079) Testosterone replacement is "fountain of youth" for men [Last Updated On: January 3rd, 2018] [Originally Added On: July 27th, 2012]
- 0080) Pill for low testosterone in men heads for phase II clinical trials [Last Updated On: December 31st, 2017] [Originally Added On: August 2nd, 2012]
Word Count: 1078