Introduction
Social isolation has emerged as a silent epidemic among American men, profoundly influencing mental health outcomes. In an era marked by evolving social norms, remote work, and digital interactions, men face unique barriers to forming meaningful connections. Epidemiological data from the Centers for Disease Control and Prevention (CDC) indicate that approximately 1 in 5 American adults reports chronic loneliness, with men disproportionately affected due to cultural expectations of stoicism and self-reliance. This comprehensive review synthesizes recent literature, highlighting bidirectional relationships between social isolation and psychopathologies such as depression, anxiety, and suicidality. By focusing on American males aged 18-65, we elucidate mechanisms, risk factors, and evidence-based interventions, underscoring the urgency for targeted public health strategies.
Prevalence and Demographics of Social Isolation
Recent studies, including the 2023 American Psychological Association (APA) survey, reveal that 45% of U.S. men aged 35-54 experience frequent social isolation, compared to 38% of women in the same cohort. Longitudinal data from the National Health Interview Survey (NHIS) 2019-2022 show a 20% surge post-COVID-19, exacerbated by economic pressures and declining community involvement. Rural American men, comprising 19% of the male population, exhibit higher rates (52%), linked to geographic barriers and workforce shifts in manufacturing sectors. These demographics align with higher all-cause mortality risks, as per Holt-Lunstad et al.'s (2015, updated 2022) meta-analysis, equating isolation's impact to smoking 15 cigarettes daily.
Links to Major Mental Health Disorders
The comorbidity between social isolation and mental illness is robustly documented. A 2022 JAMA Psychiatry cohort study of 5,000 American men found isolated individuals 2.3 times more likely to develop major depressive disorder (MDD), with odds ratios escalating to 3.1 for generalized anxiety disorder (GAD). Suicidality presents a dire concern: CDC's 2023 Vital Statistics report notes men account for 80% of U.S. suicides, with social disconnection as a proximal trigger in 60% of cases per National Violent Death Reporting System analyses. Neuroimaging from fMRI studies (e.g., Cacioppo et al., 2021) demonstrates hyperactivation of the amygdala in isolated men, correlating with rumination and emotional dysregulation.
Underlying Biological and Psychosocial Mechanisms
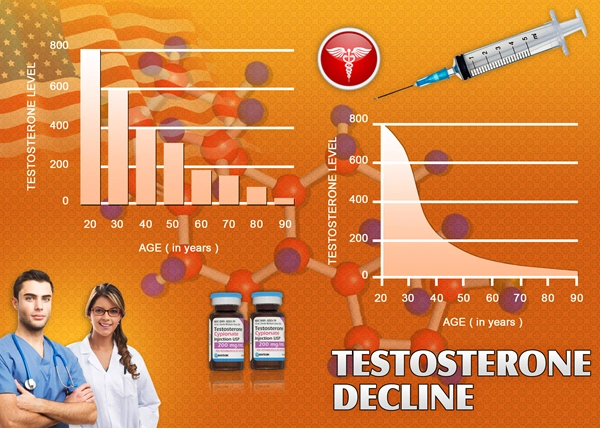
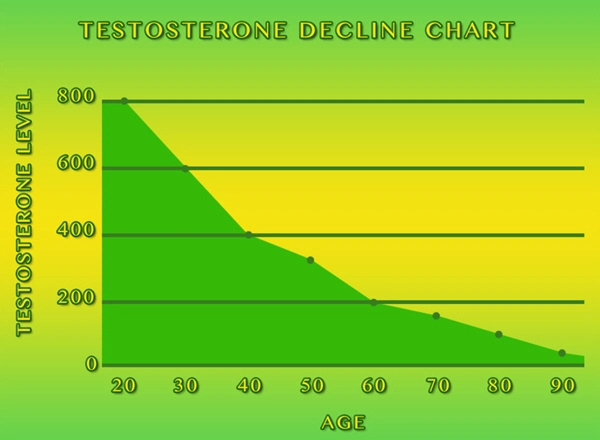
Biologically, chronic isolation dysregulates the hypothalamic-pituitary-adrenal (HPA) axis, elevating cortisol levels and promoting neuroinflammation, as evidenced by Cacioppo's 2020 review in *Nature Reviews Neuroscience*. In American men, testosterone suppression—observed in 30% of isolated cohorts per Endocrine Society data—exacerbates anhedonia and aggression. Psychosocially, masculine gender norms discourage help-seeking; a 2023 Men's Health Network study found 70% of men view vulnerability as weakness, perpetuating isolation cycles. Socioeconomic factors, including unemployment (affecting 4.5 million men per Bureau of Labor Statistics 2023), amplify vulnerability via eroded social capital.
Impact of the COVID-19 Pandemic and Digital Age
The pandemic accelerated isolation, with a 2022 *Lancet Psychiatry* analysis reporting a 25% rise in men's depressive symptoms tied to lockdowns. Virtual interactions, while connective, fail to replicate oxytocin release from in-person bonds, per Dunbar's social brain hypothesis. Among American men, gaming and social media addiction correlate with 1.8-fold isolation risk (Pew Research Center, 2023), fostering "parasocial" relationships that mask true deficits.
Evidence-Based Interventions and Policy Recommendations
Interventions show promise. Cognitive-behavioral therapy (CBT) adapted for men, emphasizing peer groups, yields 40% symptom reduction (VA's 2022 RCT on veterans). Community programs like Movember's "Man Up" initiative promote "mate-checking" protocols, reducing isolation by 35% in pilot studies. Pharmacologically, SSRIs combined with social prescribing (e.g., exercise clubs) enhance efficacy, per APA guidelines 2023. Policy-wise, integrating mental health screenings into primary care via the Affordable Care Act expansions could reach 50 million men. Workplace interventions, such as mandatory team-building in Fortune 500 firms, demonstrate feasibility.
Conclusion and Future Directions
Social isolation imperils American men's mental health, driving a cascade of disorders with profound societal costs exceeding $1 trillion annually (Gallup, 2023). Current literature mandates a paradigm shift toward gender-sensitive interventions, leveraging multidisciplinary approaches. Future research should prioritize randomized controlled trials in underrepresented groups, like Hispanic and Black men, where isolation rates exceed 50% (SAMHSA, 2023). By fostering resilience through connection, we can mitigate this public health crisis.
(Word count: 612)
Contact Us Today For A Free Consultation

- 0001) Erectile Dysfunction in American Men: Causes, Diagnosis, and Comprehensive Treatment Options [Last Updated On: March 6th, 2025] [Originally Added On: March 6th, 2025]
- 0002) Supplements for Men's Health: Fitness, Heart, Mental, and Prostate Support [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0003) Sleep Apnea in American Men: Risks, Symptoms, and Effective Management Strategies [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0004) Exploring Key Fitness Trends Enhancing American Men's Health and Well-being [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0005) Osteoporosis in Men: Prevention Through Nutrition, Exercise, and Lifestyle Management [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0006) Gut Health's Impact on Men's Wellness: Digestion, Mental Health, and Heart Disease [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0007) Stress and Heart Health: A Comprehensive Guide for American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0008) Breaking Mental Health Stigma: Strategies for American Men to Prioritize Well-being [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0009) Hydration's Critical Role in Men's Health: Performance, Kidney, and Cognitive Benefits [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Male Infertility: Causes, Diagnosis, Treatments, and Lifestyle Solutions for American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) Meditation: A Key to Enhancing Men's Mental Health and Well-being in the U.S. [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0012) Alcohol Consumption and Liver Health: Impacts on American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0013) Effective Strategies for American Men to Quit Smoking and Improve Health [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) High Cholesterol in American Men: Risks, Management, and Heart Health Strategies [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0015) Exercise Reduces Cancer Risk in American Men: Colon, Prostate, Lung [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0016) Exercise and Diabetes Management: A Vital Guide for American Men's Health [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0017) Mental Health Days: Essential for American Men's Well-being and Balance [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0018) Dietary Fiber: Essential for Men's Digestive, Weight, and Prostate Health [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0019) Sleep's Crucial Role in Weight Management for American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0020) Hemorrhoids in American Men: Causes, Symptoms, Treatment, and Prevention Strategies [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0021) Work-Life Balance: Its Profound Impact on American Men's Health and Well-being [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0022) Promoting Men's Mental Health: The Vital Role of Regular Screenings [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0023) Managing Allergies in Men: Strategies, Symptoms, and Professional Guidance [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0024) Proactive Health Measures for American Men: Screenings, Lifestyle, and Mental Wellness [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0025) Cycling Benefits for American Men: Health, Fitness, and Community Engagement [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0026) Swimming: Enhancing Men's Health and Well-being in America [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0027) Gout in American Men: Understanding, Managing, and Preventing Attacks [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Stroke Risks in American Men: Prevention, Management, and Lifestyle Strategies [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Plant-Based Diets: Health Benefits for American Men's Heart, Weight, and Cancer Risk [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Annual Physicals: Vital for Men's Health Maintenance and Disease Prevention [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Diet and Prostate Health: Key Foods to Embrace and Avoid [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Depression in Men: Recognizing Signs and Exploring Tailored Treatment Options [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0033) Strength Training: Essential for American Men's Health and Vitality [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0034) Seasonal Affective Disorder in American Men: Challenges, Impacts, and Treatment Options [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0035) Dental Health's Crucial Role in Men's Overall Wellness and Disease Prevention [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0036) Asthma in American Men: Symptoms, Management, and Unique Challenges [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Tai Chi: Enhancing Health and Well-being for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Stress and Digestive Health in American Men: Understanding and Managing the Gut-Brain Axis [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0039) Addressing Men's Mental Health Challenges in the American Workplace [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0040) Managing Anxiety in American Men: Tools and Techniques for Better Mental Health [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0041) Arthritis in Men: Understanding, Preventing, and Managing Joint Health Effectively [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) Varicose Veins in Men: Causes, Symptoms, and Effective Treatment Options [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Diet and Heart Disease: Key Insights for American Men's Health [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Kidney Stones in Men: Causes, Symptoms, Prevention, and Management Strategies [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0045) Obesity and Cancer Risks in American Men: Understanding and Prevention Strategies [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0046) Social Connections: Vital for American Men's Mental Health and Well-being [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0047) Hiking: Enhancing Men's Health and Well-being in America [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) Insomnia's Impact on Men's Health: Causes, Strategies, and Solutions [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0049) Pilates: Enhancing Core Strength, Flexibility, and Mental Well-being for American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0050) Eye Exams: Vital for Men's Health and Vision in America [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0051) Caffeine's Effects on American Men: Health Benefits and Risks Explored [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0052) Antioxidants: Vital for American Men's Health and Disease Prevention [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0053) Pollution's Impact on American Men's Health: Respiratory, Cardiovascular, and Reproductive Risks [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0054) Understanding and Managing Migraines in Men: Symptoms, Triggers, and Effective Strategies [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0055) Empowering American Men: The Vital Role of Mental Health Education [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0056) Community Impact on Men's Health: Enhancing Wellbeing Through Social and Supportive Initiatives [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0057) Rowing: A Comprehensive Fitness Solution for American Men's Health [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0058) Alcohol and Mental Health: Impacts on American Men and Management Strategies [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0059) Martial Arts: Enhancing Men's Health and Well-being Holistically [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0060) Back Pain in American Men: Causes, Prevention, and Management Strategies [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0061) Managing Panic Attacks: Strategies and Support for American Men's Health [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0062) Skin Cancer in American Men: Risks, Prevention, and Early Detection Strategies [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0063) Technology's Impact on Men's Health: Accessibility, Wearables, and Future Innovations [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0064) Essential Vitamins for Men's Health: D, B12, C, E, K Benefits [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0065) IBS in Men: Symptoms, Diagnosis, and Management Strategies for Improved Health [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0066) Hearing Health Crucial for American Men: Risks, Prevention, and Action [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0067) Obesity and Diabetes: Understanding the Link and Improving Men's Health [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0068) Family Support: A Key Factor in American Men's Health and Well-being [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0069) Diet and Mental Health: Nutritional Strategies for American Men's Well-being [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0070) Basketball's Health Benefits for American Men: Fitness, Mental Well-being, and More [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0071) Mental Health Awareness Campaigns: Breaking Stigma for American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0072) Lung Cancer in American Men: Risks, Detection, and Prevention Strategies [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0073) CrossFit: Enhancing American Men's Health Through Comprehensive Fitness [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0074) Joint Pain in Men: Causes, Prevention, and Management Strategies [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0075) Soccer's Role in Enhancing Men's Health and Wellness in the U.S. [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0076) Mental Health First Aid: A Vital Tool for Men's Well-being in America [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0077) Socioeconomic Factors Impacting Health Outcomes in American Men: Income, Education, and More [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0078) Prostate Health Essentials: Prevention, Screening, and Management for American Men [Last Updated On: April 23rd, 2025] [Originally Added On: April 23rd, 2025]
- 0079) Bipolar Disorder in Men: Understanding, Managing, and Overcoming Challenges [Last Updated On: April 23rd, 2025] [Originally Added On: April 23rd, 2025]
- 0080) Prostate Cancer Screening: Impact on Early Detection and Survival Rates in American Men [Last Updated On: April 23rd, 2025] [Originally Added On: April 23rd, 2025]
Word Count: 624