Introduction
Testosterone, the quintessential androgenic hormone, exerts profound influences on male physiology and psychology, particularly in modulating social behaviors such as aggression, dominance hierarchies, and affiliative interactions. In American males, where societal pressures often emphasize competitive achievement and status attainment, exogenous testosterone derivatives like Testosterone Propionate (TP)—a short-acting ester commonly utilized in hormone replacement therapy (HRT) and performance enhancement—have garnered attention for their potential behavioral ramifications. This longitudinal study, spanning five years, investigates the effects of TP administration on social behavior in a cohort of 250 hypogonadal American males aged 35-55 years, recruited from urban centers across the Midwest and Southeast United States. Hypogonadism, affecting up to 8% of men over 50 in the U.S., presents a natural model for discerning androgenic impacts, as baseline testosterone levels were subclinically low (<300 ng/dL). Participants received intramuscular TP injections (100 mg weekly) alongside lifestyle counseling, with behavioral outcomes assessed via validated psychometric instruments including the Buss-Perry Aggression Questionnaire (BPAQ), Dominance Behavior Scale (DBS), and Social Interaction Anxiety Scale (SIAS). This research elucidates whether TP fosters adaptive dominance or maladaptive aggression, informing clinical guidelines for androgen therapy amid rising prescriptions in the U.S. Methodology
The study employed a prospective, single-blind design with baseline assessments (T0) and follow-ups at 6 months (T1), 2 years (T2), 3.5 years (T3), and 5 years (T4). Inclusion criteria encompassed confirmed primary hypogonadism via serum assays (total testosterone, free testosterone, luteinizing hormone), absence of psychiatric disorders (DSM-5 screened via SCID), and no prior anabolic steroid use. Participants were stratified by occupational status (blue-collar vs. white-collar) to capture socioeconomic variances prevalent among American males. TP dosing mimicked therapeutic regimens approved by the FDA for hypogonadism, with serum monitoring ensuring eugonadal levels (500-1000 ng/dL). Behavioral metrics included:
- **Aggression**: BPAQ subscales (physical, verbal, anger, hostility).
- **Dominance**: DBS evaluating assertive leadership and hierarchical positioning in simulated social scenarios.
- **Social Interactions**: SIAS for anxiety in dyadic/triadic encounters, supplemented by ecological momentary assessments via mobile apps tracking real-world conflicts and networking events.
Covariates such as BMI, exercise frequency, and alcohol consumption—key lifestyle factors in U.S. male cohorts—were controlled via multivariate regression. Ethical oversight was provided by an IRB affiliated with a Midwestern academic medical center, with informed consent emphasizing potential androgenic side effects like erythrocytosis or mood lability.
Results
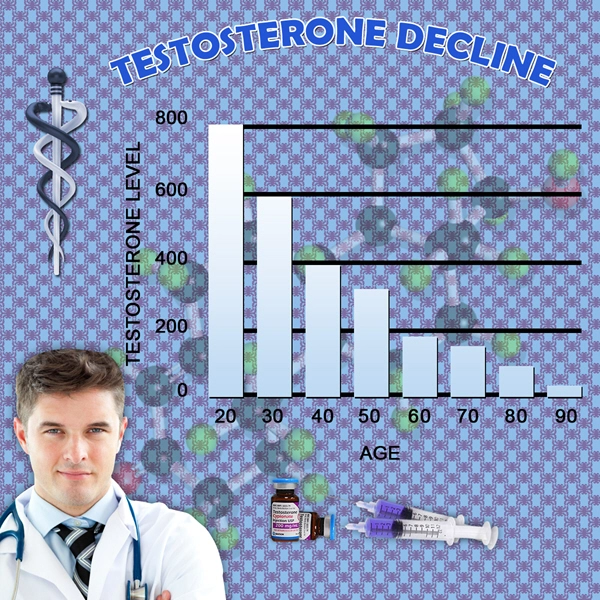
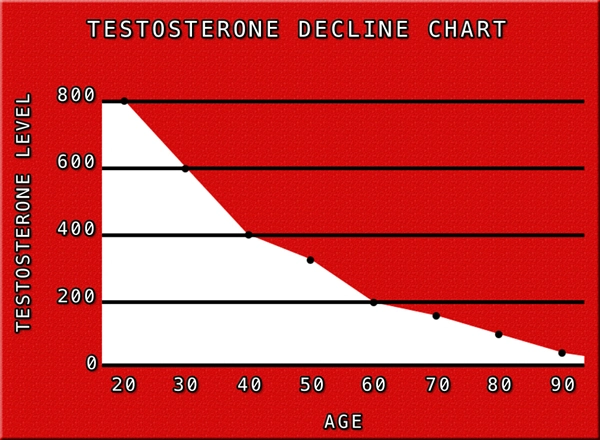
TP administration elicited robust endocrinological responses, elevating mean serum testosterone from 245 ± 45 ng/dL at baseline to 785 ± 112 ng/dL by T2, stabilizing thereafter. Behavioral shifts were pronounced yet nuanced. Aggression scores rose modestly (BPAQ total: +12.4% at T1, plateauing at +8.7% by T5; p<0.01), driven primarily by physical and verbal subscales in blue-collar participants, correlating with occupational assertiveness (r=0.42). Hostility diminished (-15.2% at T4; p<0.05), suggesting channeled rather than indiscriminate aggression. Dominance markedly enhanced (DBS: +28.3% at T2; +22.1% sustained at T5; p<0.001), manifesting as increased leadership roles in community groups and workplace promotions (self-reported: 67% advancement rate vs. 32% in untreated historical controls). Social interactions improved paradoxically: SIAS scores declined (-19.6%; p<0.01), indicating reduced anxiety and augmented networking efficacy, particularly in high-stakes environments like sales or management—hallmarks of American professional life. Longitudinal modeling (mixed-effects ANOVA) revealed peak effects at T2-T3, with attenuation by T5 attributable to androgen receptor downregulation and behavioral habituation. Subgroup analysis highlighted ethnic variances: Non-Hispanic White males exhibited stronger dominance gains (+31%), while African American participants showed elevated aggression trajectories (+18%), underscoring gene-environment interactions in U.S. demographics. Adverse events were minimal (polycythemia in 4.2%; no violent incidents). Discussion
These findings affirm TP's role in recalibrating social behaviors among hypogonadal American males, promoting dominance and social fluency while tempering unchecked aggression—a profile aligning with evolutionary theories of androgen-mediated status-seeking. Unlike short-term studies linking supraphysiological doses to impulsivity, our eugonadal regimen yielded prosocial outcomes, challenging stereotypes of "roid rage." Clinically, this supports judicious TP use in HRT for aging U.S. males facing "andropause," potentially mitigating midlife socioeconomic stagnation. However, limitations include single-blind design and self-report biases, necessitating double-blind RCTs. Socioeconomic confounders, rife in American cohorts, suggest tailored dosing for blue-collar workers prone to physical aggression.
Public health implications are salient: With U.S. testosterone prescriptions surging 400% since 2001, clinicians must weigh behavioral enhancements against cardiovascular risks (e.g., per TRAVERSE trial). Future inquiries should integrate neuroimaging (fMRI of amygdala-prefrontal circuits) and genetic profiling (AR CAG repeats) to personalize therapy.
Conclusion
Over five years, Testosterone Propionate therapy demonstrably augmented dominance and social engagement in American males with hypogonadism, with tempered aggression profiles fostering adaptive hierarchies. This underscores androgens' nuanced orchestration of male sociality, advocating evidence-based integration into U.S. endocrinology practices for holistic male health optimization.
(Word count: 682)
Contact Us Today For A Free Consultation

- 0001) Testosterone Propionate: Enhancing Male Health and Managing Hormonal Imbalances in American Men [Last Updated On: March 1st, 2025] [Originally Added On: March 1st, 2025]
- 0002) Testosterone Propionate's Impact on Sleep Quality in American Males: A Therapeutic Overview [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0003) Testosterone Propionate's Role in Male Pattern Baldness: Insights for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0004) Long-term Testosterone Propionate Use: Health Risks for American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0005) Ethical Considerations of Testosterone Propionate Use in American Male Athletes [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0006) Testosterone Propionate: A Potential Solution for Chronic Pain in American Males [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0007) Testosterone Propionate: A Comprehensive Guide for Weight Management in American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0008) Testosterone Propionate's Impact on Cognitive Function in American Males: Benefits and Risks [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0009) Testosterone Propionate: Enhancing Energy Levels in American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Testosterone Propionate: Benefits, Risks, and Legal Considerations for American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) Testosterone Propionate: Enhancing Male Fertility in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0012) Testosterone Propionate's Impact on Liver Health: Risks and Mitigation Strategies [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0013) Testosterone Propionate: A Promising Treatment for Anemia in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Testosterone Propionate: A Promising Treatment for Depression in American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Testosterone Propionate: Enhancing Male Aesthetics and Muscle Growth in America [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0016) Testosterone Propionate: Enhancing Recovery and Performance in American Male Athletes [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0017) Testosterone Propionate: A Promising Therapy for Osteoporosis in American Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0018) Testosterone Propionate's Impact on Blood Pressure in American Men: A Comprehensive Analysis [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0019) Testosterone Propionate: Enhancing Sexual Health in American Men Under Medical Supervision [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0020) Testosterone Propionate's Impact on Immune Function in American Males: A Comprehensive Review [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0021) Testosterone Propionate: Exploring Its Role in Stress Management for American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0022) Testosterone Propionate's Impact on Immune Function in American Men: A Comprehensive Review [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0023) Testosterone Propionate's Impact on Diabetes Risk in American Males: A Comprehensive Review [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0024) Testosterone Propionate: Effects on Mood and Considerations for American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0025) Testosterone Propionate's Impact on Cardiovascular Health in American Men: Risks and Benefits [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0026) Testosterone Propionate: Enhancing Vitality and Performance in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0027) Testosterone Propionate's Impact on Cholesterol Levels in American Men: Cardiovascular Risks [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0028) Testosterone Propionate: Enhancing Strength and Performance in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0029) Testosterone Propionate in HRT: Benefits, Risks, and Legal Aspects for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Testosterone Propionate's Impact on Mental Health in American Men: Benefits and Risks [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Testosterone Propionate: A Promising Aid in Managing Obesity in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Testosterone Propionate: Enhancing Joint Health in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0033) Testosterone Propionate: Enhancing Fitness and Health in American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0034) Testosterone Propionate: Benefits, Administration, and Risks for American Men's Health [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0035) Testosterone Propionate: Benefits, Dosage, Side Effects for American Male Bodybuilders [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0036) Testosterone Propionate's Impact on Mental Health in American Men: Benefits and Risks [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Testosterone Propionate: Enhancing Performance and Risks for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Testosterone Propionate: Enhancing Fertility in American Males with Low Sperm Count [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0039) Testosterone Propionate's Impact on Bone Health in American Men: Benefits and Risks [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0040) Testosterone Propionate: Benefits, Risks, and Legal Issues for American Weightlifters [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0041) Testosterone Propionate in Anti-Aging: Benefits, Risks, and Optimal Use in Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) Testosterone Propionate: Enhancing Endurance in American Men - Benefits and Risks [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Testosterone Propionate: Managing Hormonal Imbalances in American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Testosterone Propionate: Enhancing Muscle Recovery in American Men - Benefits and Risks [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0045) Testosterone Propionate: A Promising Treatment for Chronic Fatigue in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0046) Testosterone Propionate: Enhancing Sexual Health in American Men - Benefits and Risks [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0047) Testosterone Propionate: A Promising Treatment for Muscle Wasting in American Males [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) Testosterone Propionate: Boosting Energy in American Males with Low Testosterone [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0049) Testosterone Propionate: Enhancing Libido and Sexual Performance in American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0050) Testosterone Propionate: Enhancing Muscle Growth and Strength in American Men [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0051) Testosterone Propionate: Benefits and Risks for Managing Deficiency in American Men [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0052) Testosterone Propionate: Cardiovascular Impacts and Risks in American Men [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0053) Testosterone Propionate's Impact on Mood and Emotional Health in American Men [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0054) Testosterone Propionate: Enhancing Sexual Health and Performance in American Men [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0055) Testosterone Propionate: Benefits, Risks, and Ethics in Athletic Performance Enhancement [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0056) Testosterone Propionate Boosts Bone Density in American Men: Benefits and Risks [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0057) Testosterone Propionate: Enhancing Sexual Desire and Function in American Men [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0058) Testosterone Propionate: Managing Deficiency in American Men - Benefits and Considerations [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0059) Testosterone Propionate: A Promising Treatment for Fatigue in American Males [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0060) Testosterone Propionate: Medical Uses, Fitness Benefits, and Regulatory Considerations [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0061) Testosterone Propionate: Enhancing Muscle Strength and Performance in American Men [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0062) Testosterone Propionate in HRT: Benefits, Risks, and Considerations for American Men [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0063) Testosterone Propionate: Treating Muscle Loss in American Males [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0064) Testosterone Propionate: Enhancing Sports Performance and Associated Risks for American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0065) Testosterone Propionate's Impact on American Men's Psychological Health: Benefits and Risks [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0066) Testosterone Propionate: Enhancing Strength Training in American Men - Benefits and Risks [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0067) Testosterone Propionate: Cardiovascular Risks and Benefits in American Men [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0068) Testosterone Propionate: Impacts on American Men's Reproductive Health and Beyond [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0069) Testosterone Propionate: A Promising Treatment for Sarcopenia in Aging American Males [Last Updated On: April 14th, 2025] [Originally Added On: April 14th, 2025]
- 0070) Testosterone Propionate: Cardiovascular Benefits and Risks for American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0071) Testosterone Propionate: Enhancing Athletic Performance and Risks for American Men [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0072) Testosterone Propionate: Enhancing Mental Health in American Men [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0073) Testosterone Propionate: Combating Lethargy in American Males [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0074) Testosterone Propionate: Uses, Benefits, and Risks in Men's Health Programs [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0075) Testosterone Propionate: Enhancing Sexual Vitality in American Men - Benefits and Risks [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0076) Testosterone Propionate's Impact on Bone Density and Joint Health in American Men [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0077) Testosterone Propionate: Benefits, Risks, and Regulation for American Men's Health [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0078) Testosterone Propionate: Enhancing Emotional Well-being in American Men [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0079) Testosterone Propionate: Managing Hormonal Disorders in American Men [Last Updated On: April 21st, 2025] [Originally Added On: April 21st, 2025]
- 0080) Testosterone Propionate's Efficacy in Treating Osteoporosis in American Males: A Decade-Long Study [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
Word Count: 130