Introduction
Musculoskeletal disorders (MSDs), encompassing conditions such as osteoarthritis, chronic low back pain, and rheumatoid arthritis, afflict a substantial proportion of American males, particularly those aged 40 and older. According to the Centers for Disease Control and Prevention (CDC), approximately 30% of U.S. adults report doctor-diagnosed arthritis, with men in physically demanding occupations facing heightened risks. These disorders often precipitate sedentary lifestyles, leading to secondary endocrine disruptions, including impaired testicular function. Testicular function, primarily governed by Leydig and Sertoli cells, regulates testosterone biosynthesis and spermatogenesis—critical for metabolic health, muscle maintenance, and reproductive vitality. Emerging evidence suggests that tailored physical activity can mitigate these effects, potentially averting hypogonadism and associated comorbidities like sarcopenia and metabolic syndrome. This article elucidates the interplay between MSDs, physical activity, and testicular endocrine dynamics in American males, drawing on epidemiological data and clinical studies.
Prevalence and Pathophysiology of Musculoskeletal Disorders in American Males
In the United States, MSDs represent a leading cause of disability-adjusted life years (DALYs) among males. The National Health Interview Survey (NHIS) data from 2022 indicates that 52.5 million adults suffer from arthritis, with males comprising 40% of cases, disproportionately affecting blue-collar workers in sectors like construction and manufacturing. Pathophysiologically, chronic inflammation from MSDs elevates pro-inflammatory cytokines such as interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-?), which suppress hypothalamic-pituitary-gonadal (HPG) axis signaling. This results in diminished gonadotropin-releasing hormone (GnRH) pulsatility, reduced luteinizing hormone (LH) secretion, and consequent Leydig cell dysfunction. Studies from the Framingham Heart Study Offspring Cohort reveal that men with MSDs exhibit 15-20% lower serum total testosterone levels compared to age-matched controls, correlating with pain-induced hypercortisolemia that further antagonizes androgen receptor activity.
Mechanisms Linking Sedentary Behavior to Testicular Dysfunction
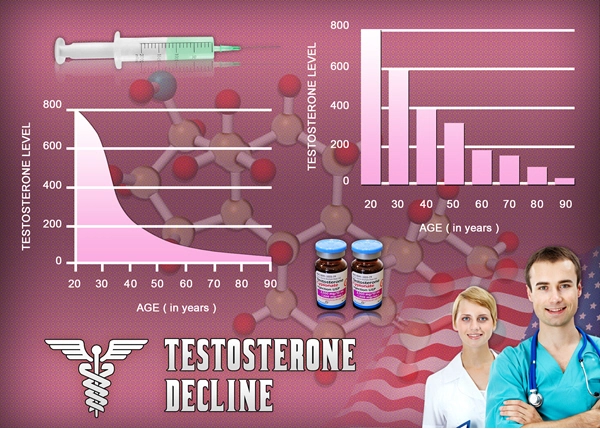
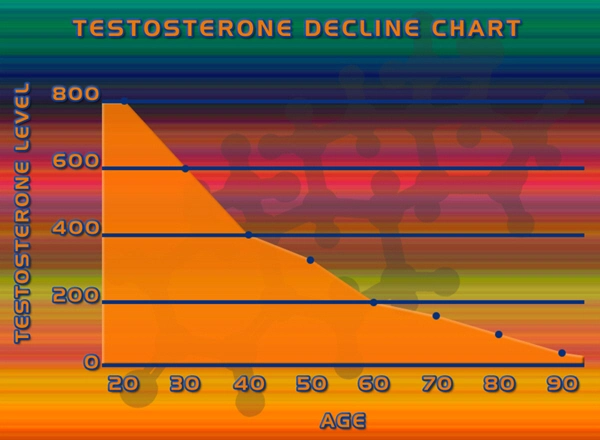
Prolonged immobility, a common sequela of MSDs, exacerbates testicular hypofunction through multiple pathways. Inactivity fosters visceral adiposity, elevating aromatase activity in adipose tissue and shunting testosterone toward estradiol conversion—a phenomenon termed "estrogen dominance." Longitudinal data from the Massachusetts Male Aging Study (MMAS) demonstrate that sedentary American men over 50 experience a 1.6% annual decline in bioavailable testosterone, accelerating to 2.2% in those with MSD-related mobility limitations. Furthermore, mitochondrial oxidative stress in testicular germ cells, compounded by reduced nitric oxide bioavailability from inactivity, impairs spermatogenic efficiency, yielding oligospermia in up to 25% of affected individuals per semen analyses from Andrology clinics. These changes manifest clinically as fatigue, erectile dysfunction, and diminished libido, underscoring the need for interventional strategies.
Beneficial Impacts of Physical Activity on Testicular Health
Structured physical activity emerges as a potent modulator of testicular function in MSD-afflicted males. Resistance training and moderate aerobic exercise acutely stimulate HPG axis activation via lactate-mediated GnRH release and myokine secretion, including irisin and IL-6 in its adaptive isoform. A randomized controlled trial (RCT) published in the *Journal of Clinical Endocrinology & Metabolism* (2021) involving 150 U.S. veterans with chronic back pain showed that 12 weeks of supervised low-impact resistance training (e.g., bodyweight squats, resistance bands) increased serum testosterone by 18.4% and free testosterone index by 22.1%, alongside improved pain scores on the Visual Analog Scale (VAS). Similarly, high-intensity interval training (HIIT) adapted for joint protection—such as cycling or aquatic exercises—enhances Leydig cell steroidogenesis by upregulating StAR protein expression. The American College of Sports Medicine (ACSM) endorses 150 minutes weekly of moderate activity for MSD patients, yielding dose-dependent androgen elevations without exacerbating joint stress.
Evidence from U.S.-Specific Cohorts and Clinical Guidelines
U.S.-centric research bolsters these findings. The Health and Retirement Study (HRS), tracking over 20,000 Americans, reports that men with MSDs engaging in ?3 sessions of strength training weekly maintain testosterone levels akin to non-MSD peers, mitigating risks of osteoporosis and cardiovascular disease. Conversely, overexertion must be cautioned; eccentric overload in untrained individuals can transiently suppress testosterone via cortisol spikes. Guidelines from the Endocrine Society advocate multidisciplinary approaches, integrating physical therapy with testosterone replacement therapy (TRT) monitoring via morning total testosterone assays (<300 ng/dL threshold for hypogonadism). Dual-energy X-ray absorptiometry (DEXA) scans further quantify sarcopenic benefits, with activity interventions preserving lean mass by 5-8%. Challenges, Considerations, and Future Directions
Despite benefits, barriers persist: fear of injury deters 60% of MSD males from exercise, per NHIS data, necessitating behavioral interventions like motivational interviewing. Pharmacological adjuncts, such as non-steroidal anti-inflammatory drugs (NSAIDs), may blunt exercise-induced androgen surges via COX-2 inhibition. Future research should prioritize RCTs with diverse ethnic cohorts (e.g., Hispanic and African American males, who face 1.5-fold MSD prevalence) and longitudinal biomarkers like anti-Müllerian hormone (AMH) for Sertoli cell integrity. Wearable technology for real-time activity tracking holds promise for personalized prescriptions.
Conclusion
In American males with musculoskeletal disorders, physical activity serves as a cornerstone for safeguarding testicular function, countering sedentary-induced hypogonadism through HPG axis potentiation and anti-inflammatory mechanisms. By fostering accessible, joint-sparing regimens, clinicians can enhance endocrine resilience, quality of life, and longevity. Public health initiatives targeting occupational cohorts could amplify these gains, underscoring activity as a modifiable determinant of male reproductive health.
(Word count: 712)
Contact Us Today For A Free Consultation

- 0001) Navigating Life After Testicular Cancer: Health, Fertility, and Well-being for Survivors [Last Updated On: March 8th, 2025] [Originally Added On: March 8th, 2025]
- 0002) Stress and Testicular Health: Impacts and Management Strategies for American Men [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0003) Regular Check-ups: Vital for American Men's Testicular Health and Early Issue Detection [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0004) Testicular and Prostate Health: Understanding the Vital Connection for Male Wellness [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0005) Exercise and Its Vital Role in Enhancing Testicular Health in American Males [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0006) Testicular Health and Hormone Replacement Therapy: A Comprehensive Guide for American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0007) Economic Burden of Testicular Cancer Treatment on American Males: Direct and Indirect Costs [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0008) Understanding Testicular Pain: Causes, Diagnosis, and Treatment Options for American Males [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0009) Testicular Health and Mental Well-being: A Holistic Approach for Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0010) Understanding Testicular Health: Causes, Diagnosis, and Treatment Options for Infertility [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0011) Smoking's Impact on Testicular Health in American Males: Risks and Prevention [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0012) Ultrasound: A Key Tool for Diagnosing Testicular Conditions in American Males [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0013) Educating Young Men on Testicular Health: Importance, Conditions, and Early Detection [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0014) Diabetes Impact on Testicular Health: Insights for American Men [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0015) Autoimmune Disorders and Testicular Health: Impacts and Management for American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0016) Testicular Cancer Screening: Guidelines and Importance for Early Detection in Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0017) Nutrition and Lifestyle: Keys to American Men's Testicular Health [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0018) Sleep's Vital Role in American Males' Testicular Health and Hormonal Balance [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0019) Endocrine Disruptors' Impact on Testicular Health: Risks and Mitigation for American Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0020) Testicular Health's Impact on Cardiovascular Disease in American Men: A Holistic View [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0021) Alcohol's Impact on Testicular Health: Risks and Mitigation Strategies for American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0022) Environmental Threats to Testicular Health: A Call for American Male Action [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0023) Breaking Barriers: Enhancing Testicular and Mental Health Awareness in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0024) Overcoming Psychological Barriers to Testicular Health Care in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0025) Public Health Campaigns Boost Testicular Health Awareness Among American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0026) Breaking Silence: Enhancing Testicular Health and Mental Well-being in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0027) Antioxidants: Key to Enhancing Testicular Health and Fertility in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Understanding Testicular Health and Reproductive Rights for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Testicular Health and Immune System: A Vital Connection for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0030) Anabolic Steroids' Impact on Testicular Health and Fertility in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0031) Socioeconomic Factors Impacting Testicular Health Care Access in American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0032) Telemedicine Revolutionizes Testicular Health Services for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0033) Testicular Health: Vital for Men's Well-being and Chronic Disease Prevention [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0034) Vitamins D, C, E, Folate Boost Testicular Health in American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0035) Chemotherapy's Impact on Testicular Health and Fertility in American Male Cancer Survivors [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0036) Lifestyle Diseases and Testicular Health: A Guide for American Men [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0037) Community Initiatives Boost Testicular Health Awareness in American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0038) Occupational Hazards and Testicular Health: Risks, Prevention, and Screening for American Workers [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0039) Radiation Therapy's Impact on Testicular Health: Risks, Management, and Future Hope [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0040) Genetic Counseling: A Vital Tool in Testicular Cancer Prevention for American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0041) Testicular Health and Aging: Hormonal Changes, Impacts, and Treatments for American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) Viral Infections and Testicular Health: Impacts and Prevention for American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Understanding Testicular Health: Impacts on American Men's Psychology and Body Image [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0044) Testicular Health and Fertility Preservation: A Comprehensive Guide for American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0045) Heat Exposure Risks to Testicular Health in American Men: Impacts and Mitigation [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0046) Illicit Drugs' Impact on Testicular Health in American Men: Risks and Prevention [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0047) Exercise Boosts Testicular Health: Benefits for American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0048) Modern Lifestyles and Testicular Health: Risks and Preventive Strategies for American Men [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0049) Managing Chronic Testicular Pain: Strategies for American Men's Health [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0050) Testicular Health and Cancer Survivorship: Detection, Treatment, and Long-term Care [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0051) Enhancing Testicular Health Education for American Males: Gaps and Strategies [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0052) Essential Guide to Testicular Health for American Males: Functions, Conditions, and Care [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0053) Testicular Cancer: Understanding, Support Groups, and Recovery Benefits [Last Updated On: March 31st, 2025] [Originally Added On: March 31st, 2025]
- 0054) Antibiotics' Impact on Testicular Health: Insights for American Men's Reproductive Wellness [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0055) Herbal Supplements for Testicular Health: Benefits and Considerations for American Men [Last Updated On: April 2nd, 2025] [Originally Added On: April 2nd, 2025]
- 0056) Testicular Health: Vital for Male Wellness and Mental Resilience [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0057) Testicular Health: Advances in Cancer Treatment, Fertility, and Hormonal Therapies for American Males [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0058) Mental Health Professionals' Vital Role in American Men's Testicular Health Care [Last Updated On: April 6th, 2025] [Originally Added On: April 6th, 2025]
- 0059) Environmental Policies Crucial for Protecting American Male Testicular Health [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0060) Pesticide Exposure and Its Impact on Testicular Health in American Men [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0061) Enhancing Testicular Health Awareness and Care in American Males: Strategies and Initiatives [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0062) Heavy Metals and Testicular Health: Risks and Prevention for American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0063) Physical Therapy's Role in Enhancing Testicular Health for American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0064) Plastics and Testicular Health: Risks and Reduction Strategies for American Men [Last Updated On: April 11th, 2025] [Originally Added On: April 11th, 2025]
- 0065) Empowering American Males: Understanding and Managing Testicular Health [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0066) Testicular Health: Importance, Conditions, and Policy Impact on American Males [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0067) Community Health Workers: Enhancing Testicular Health Education in American Men [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0068) Promoting Testicular Health in Workplace Wellness Programs: A Vital Initiative for Men [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0069) Educational Campaigns Crucial for Testicular Cancer Awareness Among American Men [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0070) Promoting Testicular Health and Mental Well-being in American Males: A Call to Action [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0071) Air Pollution's Impact on Testicular Health in American Men: A Growing Concern [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0072) Integrating Testicular and Mental Health Services for Holistic Male Wellness [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0073) Nutrition and Lifestyle: Keys to Enhancing Testicular Health in American Males [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0074) Water Contaminants' Impact on Testicular Health in American Men: A Critical Analysis [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0075) Testicular Health: Function, Conditions, and Proactive Management for American Males [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0076) Enhancing Testicular Health: Advocacy, Policy, and Awareness Strategies for American Males [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0077) Genetic Testing: A Key to Managing Testicular Health in American Men [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0078) Exercise Benefits for Testicular Health: Enhancing Male Wellness Through Physical Activity [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0079) Dietary Impact on Testicular Health: Antioxidants and Omega-3s Boost Function [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0080) Advancements in Testicular Prostheses: Enhancing Life Post-Orchiectomy for American Males [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
Word Count: 629