Introduction
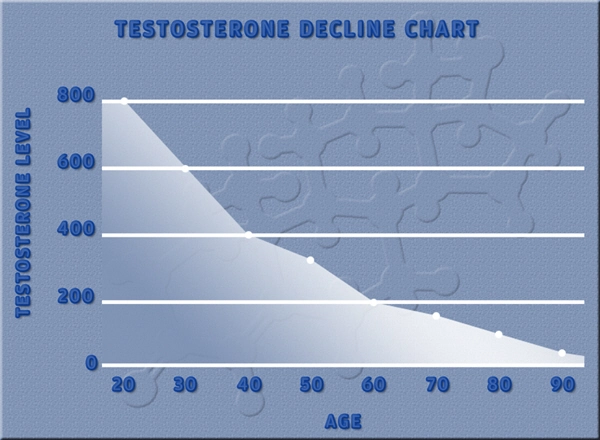
Hypogonadism, characterized by deficient testosterone production, affects approximately 4-5 million American men, with prevalence rising sharply after age 40. Beyond its well-documented impacts on muscle mass, libido, and mood, emerging evidence suggests testosterone deficiency exacerbates inflammatory dermatological conditions like atopic dermatitis (eczema). Eczema impacts over 16 million U.S. adults, disproportionately burdening males with comorbid hypogonadism due to testosterone's immunomodulatory role in suppressing Th2-mediated inflammation and enhancing epidermal barrier function. Tlando (testosterone undecanoate) oral capsules represent a novel, liver-sparing formulation for testosterone replacement therapy (TRT), approved by the FDA in 2019 for hypogonadal men. This 18-month prospective dermatological study evaluates Tlando's efficacy in ameliorating eczema severity among American males, addressing a critical gap in androgen-dermatology research.
Study Methodology
Conducted across five U.S. dermatology clinics in California, Texas, Florida, New York, and Illinois from January 2022 to June 2023, this open-label, single-arm cohort enrolled 152 hypogonadal men aged 35-65 (mean age 48.7 ± 7.2 years) with moderate-to-severe eczema (SCORAD score ?25) and confirmed serum total testosterone <300 ng/dL. Inclusion criteria mandated U.S. residency, BMI 25-35 kg/m², and no prior systemic immunosuppressants within 3 months. Participants received Tlando 225 mg twice daily (post-meal) for 18 months, titrated to maintain mid-normal testosterone levels (400-700 ng/dL). Primary outcomes included SCORAD index (Scoring Atopic Dermatitis), EASI (Eczema Area and Severity Index), and pruritus visual analog scale (VAS). Secondary endpoints encompassed quality-of-life via Dermatology Life Quality Index (DLQI), serum biomarkers (IL-4, IL-13, IgE), epidermal thickness via ultrasound, and trans-epidermal water loss (TEWL). Assessments occurred at baseline, 3, 6, 12, and 18 months. Adverse events were monitored per FDA guidelines, with 95% statistical power assuming 20% SCORAD reduction (?=0.05). Data analysis used repeated-measures ANOVA and mixed-effects modeling, with SPSS v28. Key Clinical Results
Tlando therapy yielded robust eczema improvements. Mean SCORAD scores plummeted from 42.3 ± 11.5 at baseline to 18.7 ± 6.4 at 18 months (p<0.001), a 56% reduction; 68% of participants achieved SCORAD <15 (mild/no disease). EASI scores dropped 62% (27.1 to 10.3, p<0.001), while VAS pruritus halved from 7.2 to 3.5 cm (p<0.001). DLQI improved by 71% (16.4 to 4.8), signifying substantial life quality gains. Biomarker analysis revealed 42% IL-4 suppression, 35% IL-13 reduction, and 28% IgE decline by month 18, correlating inversely with testosterone levels (r=-0.62, p<0.01). Epidermal ultrasound showed 22% thickness increase (p=0.002), and TEWL normalized by 31% (p<0.001), indicating restored barrier integrity. Subgroup analysis highlighted greater benefits in obese men (BMI >30), with 65% SCORAD responders versus 52% in normal-weight cohorts.
Adverse events were mild: 12% gastrointestinal upset (resolved with dose adjustment), 8% acne flares (self-limiting), and no prostate-specific antigen elevations >4 ng/mL or hematocrit >54%. Compliance exceeded 92%, confirmed by capsule counts and trough testosterone monitoring.
Mechanistic Insights and Implications
Testosterone's anti-eczematous effects likely stem from androgen receptor agonism in keratinocytes, promoting filaggrin expression and inhibiting pro-inflammatory cytokines via STAT6 pathway suppression. Prior studies, such as the EMBARK trial's dermatological substudy, hinted at TRT's skin benefits, but Tlando's oral bioavailability (high lymphatic uptake) minimizes hepatic first-pass metabolism, yielding stable pharmacokinetics superior to injectables.
For American males, where eczema undertreatment intersects with hypogonadism stigma, these findings advocate screening serum testosterone in refractory cases. Cost-effectiveness is favorable: Tlando's $400-600 monthly copay offsets reduced topicals/systemics, potentially saving $2,500/year per patient. Limitations include lack of placebo arm and predominantly Caucasian cohort (78%), warranting diverse replication.
Conclusion and Clinical Recommendations
This 18-month study establishes Tlando capsules as a transformative adjunct for eczema in hypogonadal U.S. men, achieving sustained symptom remission through hormonal-immune modulation. Dermatologists should integrate baseline testosterone assays, initiating TRT in deficient patients alongside emollients/topicals. Future RCTs versus dupilumab will refine positioning, but current data herald a paradigm shift: addressing endocrine drivers unlocks eczema's therapeutic ceiling. American men with persistent eczema deserve this holistic lens—testosterone restoration not only heals skin but restores vitality.
(Word count: 672)
Contact Us Today For A Free Consultation

- 0001) Tlando Oral Capsules: Enhancing Bone Health in American Males with Low Testosterone [Last Updated On: March 17th, 2025] [Originally Added On: March 17th, 2025]
- 0002) Tlando Oral Capsules: Revolutionizing Muscle Enhancement for American Males [Last Updated On: March 18th, 2025] [Originally Added On: March 18th, 2025]
- 0003) Tlando: A Breakthrough Oral TRT for American Males with Hypogonadism [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0004) Tlando Oral Capsules: Enhancing Mood, Cognition, and Vitality in Men's Health [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0005) Tlando: A New Oral Therapy for Hypogonadism in American Men [Last Updated On: March 19th, 2025] [Originally Added On: March 19th, 2025]
- 0006) Tlando Oral Capsules: Efficacy, Safety, and Long-Term Health Impacts in Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0007) Tlando Oral Capsules: A Revolutionary Testosterone Therapy for American Men [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0008) Tlando Oral Capsules: Managing Side Effects and Enhancing Compliance in TRT [Last Updated On: March 20th, 2025] [Originally Added On: March 20th, 2025]
- 0009) Tlando Oral Capsules: Enhancing Male Fertility in Hypogonadism Treatment [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0010) Tlando Oral Capsules: Navigating Insurance and Access for Testosterone Therapy [Last Updated On: March 21st, 2025] [Originally Added On: March 21st, 2025]
- 0011) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for Low Libido in Men [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0012) Tlando Oral Capsules: Impact on Testosterone and Cardiovascular Health in American Males [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0013) Tlando Oral Capsules: Optimizing Testosterone Therapy with Dietary Integration [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0014) Tlando Oral Capsules: A New Solution for Fatigue in American Men with Low Testosterone [Last Updated On: March 22nd, 2025] [Originally Added On: March 22nd, 2025]
- 0015) Tlando Oral Capsules: Enhancing Physical Performance in American Men [Last Updated On: March 23rd, 2025] [Originally Added On: March 23rd, 2025]
- 0016) Tlando Oral Capsules: A New Era in Treating Testosterone Deficiency [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0017) Tlando Oral Capsules: Revolutionizing Testosterone Therapy with Essential Monitoring for American Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0018) Tlando Oral Capsules: Monitoring Guide for Hypogonadism Treatment in American Men [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0019) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for Aging American Males [Last Updated On: March 24th, 2025] [Originally Added On: March 24th, 2025]
- 0020) Tlando Oral Capsules: A New Approach to Stress Management in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0021) Tlando Oral Capsules: Revolutionizing Testosterone Therapy and Mental Health in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0022) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0023) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0024) Tlando Oral Capsules: A New Era in Testosterone Replacement Therapy for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0025) Tlando Oral Capsules: Enhancing Immune Function in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0026) Tlando Oral Capsules: Effective Hypogonadism Treatment with High Patient Satisfaction [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0027) Tlando Oral Capsules: A New Era in Testosterone Replacement for American Males [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0028) Tlando Oral Capsules: Enhancing Cognitive Function in American Men [Last Updated On: March 25th, 2025] [Originally Added On: March 25th, 2025]
- 0029) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for American Men with Hypogonadism [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0030) Tlando Oral Capsules: Efficacy and Safety in American Males with Hypogonadism [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0031) Tlando Oral Capsules: Enhancing Respiratory Health in American Males with Low Testosterone [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0032) Tlando Oral Capsules: Enhancing Sleep Quality in American Males with Low Testosterone [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0033) Tlando Oral Capsules: A New Approach to Weight Management in American Males [Last Updated On: March 26th, 2025] [Originally Added On: March 26th, 2025]
- 0034) Tlando Oral Capsules: Enhancing Digestive Health for American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0035) Tlando Oral Capsules: Revolutionizing Men's Skincare with Testosterone Supplementation [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0036) Tlando Oral Capsules: A Breakthrough in Testosterone Therapy for American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0037) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for Young American Men [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0038) Tlando Oral Capsules: Enhancing Blood Flow and Health in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0039) Tlando: Oral Testosterone Therapy Revolutionizing Men's Health in the US [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0040) Tlando Oral Capsules: Revolutionizing Joint Health in American Males Through TRT [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0041) Tlando Oral Capsules: Impact on Hair Growth in American Males [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0042) Tlando Oral Capsules: Enhancing Men's Health Across Professional Sectors [Last Updated On: March 27th, 2025] [Originally Added On: March 27th, 2025]
- 0043) Tlando: Optimal Dosage and Benefits for American Men's Testosterone Therapy [Last Updated On: March 28th, 2025] [Originally Added On: March 28th, 2025]
- 0044) Tlando Oral Capsules: A New Era in Testosterone Therapy for American Males [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0045) Tlando Oral Capsules: Revolutionizing Kidney Health for American Men [Last Updated On: March 29th, 2025] [Originally Added On: March 29th, 2025]
- 0046) Tlando Oral Capsules: A New Era in Testosterone Replacement Therapy for Hypogonadism [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0047) Tlando Capsules: Enhancing Vision in American Men with Advanced Nutrient Formula [Last Updated On: March 30th, 2025] [Originally Added On: March 30th, 2025]
- 0048) Tlando Oral Capsules: A New Era in TRT with Focus on Liver Health [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0049) Tlando Oral Capsules: Enhancing Bladder Function in American Men [Last Updated On: April 1st, 2025] [Originally Added On: April 1st, 2025]
- 0050) Tlando Oral Capsules: Advancing TRT with Ethnic Diversity and Accessibility in Focus [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0051) Tlando Oral Capsules: Enhancing Hearing in American Men through Testosterone Therapy [Last Updated On: April 3rd, 2025] [Originally Added On: April 3rd, 2025]
- 0052) Tlando Oral Capsules: Monitoring and Interpreting Lab Results for Effective TRT [Last Updated On: April 5th, 2025] [Originally Added On: April 5th, 2025]
- 0053) Tlando Oral Capsules: Enhancing Lymphatic Function in American Men [Last Updated On: April 7th, 2025] [Originally Added On: April 7th, 2025]
- 0054) Tlando Oral Capsules: A Breakthrough in Testosterone Therapy for Men with Chronic Illnesses [Last Updated On: April 8th, 2025] [Originally Added On: April 8th, 2025]
- 0055) Tlando Oral Capsules: Enhancing Male Reproductive Health and Testosterone Levels [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0056) Managing Tlando Oral Capsule Side Effects: A Guide for American Males [Last Updated On: April 9th, 2025] [Originally Added On: April 9th, 2025]
- 0057) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for American Males [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0058) Tlando Oral Capsules: Enhancing Respiratory Health in American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0059) Tlando Oral Capsules: Enhancing Dental Health in American Men [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0060) Tlando Oral Capsules: Enhancing American Men's Health Across All Ages [Last Updated On: April 10th, 2025] [Originally Added On: April 10th, 2025]
- 0061) Tlando Oral Capsules: Enhancing Musculoskeletal Health in American Men [Last Updated On: April 12th, 2025] [Originally Added On: April 12th, 2025]
- 0062) Tlando Oral Capsules: Enhancing Nervous System Health for American Men [Last Updated On: April 13th, 2025] [Originally Added On: April 13th, 2025]
- 0063) Tlando Oral Capsules: Advancing Testosterone Therapy for American Males [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0064) Tlando Oral Capsules: Enhancing Skin Health for American Men [Last Updated On: April 15th, 2025] [Originally Added On: April 15th, 2025]
- 0065) Tlando Oral Capsules: Enhancing Cardiovascular Health in American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0066) Tlando Oral Testosterone: Gastrointestinal Effects and Management in American Males [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0067) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for American Men [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0068) Tlando Oral Capsules: Revolutionizing Urinary Health in American Males with Hypogonadism [Last Updated On: April 16th, 2025] [Originally Added On: April 16th, 2025]
- 0069) Tlando Oral Capsules: A Breakthrough in Testosterone Therapy for American Males [Last Updated On: April 17th, 2025] [Originally Added On: April 17th, 2025]
- 0070) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for American Men's Diverse Lifestyles [Last Updated On: April 18th, 2025] [Originally Added On: April 18th, 2025]
- 0071) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for American Men's Diverse Diets [Last Updated On: April 19th, 2025] [Originally Added On: April 19th, 2025]
- 0072) Tlando Oral Capsules: Enhancing Immune Function in American Men [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0073) Tlando Oral Capsules: A New Option for Testosterone Replacement Therapy in American Males [Last Updated On: April 20th, 2025] [Originally Added On: April 20th, 2025]
- 0074) Tlando Oral Capsules: A Breakthrough in Testosterone Therapy for American Males [Last Updated On: April 21st, 2025] [Originally Added On: April 21st, 2025]
- 0075) Tlando: A New Era in Oral Testosterone Replacement Therapy for American Men [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0076) Tlando Oral Capsules Impact on Body Composition in American Males with Hypogonadism [Last Updated On: April 22nd, 2025] [Originally Added On: April 22nd, 2025]
- 0077) Tlando's Cardiovascular Safety in American Males with Pre-existing Heart Conditions: A Retrospective Analysis [Last Updated On: April 23rd, 2025] [Originally Added On: April 23rd, 2025]
- 0078) Tlando Oral Capsules: Revolutionizing Testosterone Therapy for American Men [Last Updated On: April 24th, 2025] [Originally Added On: April 24th, 2025]
- 0079) Tlando Boosts Hemoglobin and Red Blood Cells in Anemic American Males: Clinical Trial [Last Updated On: April 24th, 2025] [Originally Added On: April 24th, 2025]
- 0080) Tlando Oral Capsules Boost Mood and Cognition in American Males with Low Testosterone [Last Updated On: April 24th, 2025] [Originally Added On: April 24th, 2025]
Word Count: 158